
April Falls: falls are no laughing matter

Physiotherapists are ideally placed to take a prominent role in falls prevention through education, exercise prescription and encouraging safe activity. To coincide with April Falls Week, InMotion highlights the work of just some of the clinicians and researchers at the frontline of preventing falls in the older population across three diverse settings.
Whether it is at home, in residential aged care or in the hospital setting, older Australians are at risk of experiencing a life-changing fall every day.
Falls, and their associated injuries, are often viewed by the older population as an inevitable part of the ageing process. However, physiotherapists have shown that they can be innovative in falls prevention healthcare, and are actively challenging how the profession thinks about service provision in this area.
Backed by a strong body of evidence, physiotherapists are changing the landscape in a myriad of ways to help reduce the incidence of falls by older people. From using the latest research to technological developments and innovations in exercise prescription, there is much being done behind the scenes to help patients to negotiate this sometimes rocky road.
Highlighting the steps to prevent falls in the older population during April Falls Week, and its associated month-long campaign, gives physiotherapists a platform to increase public education about falls prevention to counter the perception held by many older people that falls won‘t happen to them.
Home and community
Adelaide physiotherapist Joanna Tan, APAM, began working with a client who was 97 when he tripped on edging in his garden and took a fall. Up until that point, her client had been pretty active, but the fall knocked his confidence. Determined to remain living independently, the client took Joanna’s advice to begin using a walker for longer trips out in the community, he continued to take the bus where possible and began taking short daily walks around his neighbourhood.
Joanna visited his home and examined his environment, looked for opportunities to include exercise in her client’s activities of daily living and to work on his strength and balance. ‘He’s maintaining his volunteering at the nursing home and he catches the bus everywhere,’ Joanna says. ‘He is still living by himself, so he’s quite inspirational.’
Playing such a key role in helping her clients get back on their feet after a fall is one aspect of her work that Joanna enjoyed as a community aged care physiotherapist, one that has continued on her recent return to private practice. Throughout her career working with the older population, Joanna has seen the direct and immediate impacts a fall can have not only on the lives of her older clients but also on their families, friends and carers.

‘I found that falls are often a really big trigger for knowing that there’s a deterioration in a few aspects of someone’s life. That could be a general loss of strength, it could be they’ve had some sort of medical event such as an operation or they’ve had a stroke, or maybe they’re becoming more isolated and they’re not as active or challenging themselves anymore,’ Joanna says.
‘There are many contributing factors to a fall, which is why exploring what led to the fall is important: asking how many near misses or if they have had multiple falls over the last 12 months. Sometimes people had a fall because they are quite active and they’re out doing a lot of things and challenging themselves, and their fall may be more related to that. Generally, though, falls are a red flag for us and for medical professionals.’
In her experience, Joanna has found that many clients have been experiencing anxiety around the possibility of taking a fall long before any happenstance, triggering a chain of events that results in the older person doing less physical activity and subsequently losing strength, which in turn increases the likelihood of experiencing a fall.
She says that by honing in on what activities a client enjoys and encouraging clients to continue with those activities where possible, along with a tailored exercise program, physiotherapists can help reduce anxiety in the older population.
‘The other thing that’s quite challenging is that a realistic amount of falls prevention exercise that someone needs is quite a lot. So how do we get someone to commit to a lot of practice and attend classes? Can they afford it financially? Do they have access to transport to get there?’ Joanna says. ‘When you’re suggesting these things you also have to have some sort of way of making it realistic, and also accepting that maybe some people will not want to do that kind of activity. It is also important to follow-up with the client regularly from the falls prevention point of view, not just on their basic ache or pain or musculoskeletal injury. If there are multiple risk factors it would be worth contacting the client’s GP and considering referral to a specialised falls assessment clinic.’
During the April Falls campaign this month, Joanna will be wearing her ‘Take steps to ask me how to reduce your falls risk factor’ badge that she got a few years ago, as well as working with a dietitian in her practice to create a joint intervention that targets frailty and encourages clients to undergo a falls screening assessment.
‘I think physios have to be promoting that falls prevention is a big area that we are involved with because I know that other professions are promoting what they do— exercise physiologists are offering falls prevention exercises as well, so there is that competition in the market.
'With regards to equipment, walking aids and exercise prescription, occupational therapists are often called on for that and I think that we need to keep pushing that we’re probably better placed to determine use of walking aids and prescription of exercise. But having said that, we do still have to work with other professionals so collaborative is always best. The evidence is that multidisciplinary assessments in falls risk management is the gold standard.’
Researcher Professor Cathie Sherrington, FACP (by original contribution, as awarded by the Australian College of Physiotherapists in 2019), worked clinically for 10 years, mainly in aged care rehabilitation, before becoming interested in generating evidence to support clinical practice.
`It was frustrating to me that we didn’t always have the ability to deliver the interventions that we knew that people needed because of pressure on resources so I thought “we need to generate more evidence to support our practice”,’ Cathie says.
Cathie is well known for her systematic reviews looking at the role of exercise in falls prevention—the first in 2008 included 45 randomised controlled trials about exercise for falls prevention, and last year she and her team published a Cochrane review that had 108 randomised controlled trials of exercise for falls prevention.
‘In community-dwelling older people, it is very clear that exercise prevents falls, particularly exercise that targets balance and functional abilities through task-specific exercises,’ Cathie says. ‘Exercise like practising sit-tostand and going up steps and other activities are the bread and butter of what physios are providing and we really have strong evidence that they prevent falls.’

So how can the research be best put into practice by clinicians?
‘It’s about physios offering these type of programs themselves or finding suitable programs to refer their patients to, and encouraging those patients to go along. The evidence now is moving away from the idea of screening people for the risk of falling and just delivering exercise to the high-risk people, as we know now that everyone over 60 can actually benefit from falls prevention exercise. Physios should not just be thinking about falls in people they are seeing for falls or fractures, they should be thinking about falls prevention exercise for any person over 60.
‘Physios can work out which of their patients will need programs delivered by physios and which could go along to a community exercise program. For lower-risk people, community-type programs may be sufficient. But then a lot of physios are actually running these types of programs as well, which is fantastic.’
Cathie says the evidence shows that awareness among the general population that exercise can help prevent falls is important, as is the need for health professionals to be promoting the issues as well. ‘As physios, we need to be working with our GP colleagues and other specialists to really have them on board to be promoting appropriate exercise for falls prevention.’
Hospital
Keith Layton, APAM, is the senior physiotherapist in the older person’s evaluation, rehabilitation assessment unit at Cairns Hospital in north Queensland, and he works clinically one day a week. Concurrently, Keith also holds a clinical consultant role in the Cairns and Hinterland Hospital and Health Service’s (CHHHS) new digital system for primary health. And as the co-chair of the Cairns and Hinterland Falls Committee, Keith is among teachers who help educate the hospital wards’ dedicated ‘falls champions’ through training sessions held throughout the year.
Having previously worked in aged care and run his own business, Keith now works in the hospital’s inpatient subacute rehabilitation unit with a ‘really wonderful multidisciplinary team including geriatricians, other allied health and nursing staff’. This collegiate approach to the management of falls risk in the older population, he says, fits in with several other strategies running concurrently in the hospital, in the local health district and in the wider Queensland Health facilities.
These include:
- running strength and balance classes on the ward
- having access to a dementia delirium clinical nurse consultant at the hospital
- utilising specialised falls equipment including falls alarms integrated into beds and chair alarms for highrisk patients
- use of the Safe Recovery Program, developed by physiotherapist Professor Terry Haines
- having access to the state-wide ‘Stay on your Feet’ resource (health.qld.gov.au/stayonyourfeet)
- referring post-discharge patients on to government and non-government community services for strength and balance conditioning.
‘From an inpatients perspective, falls are a big risk factor, especially for our patients with cognitive impairment,’ Keith says. ‘After surgery there’s a high incidence of delirium, and with our older patients they may have dementia, and then there’s also a change in function, change in medications … many risk factors are there.
‘We find that [Safe Recovery Program] very effective for the cognitively intact patients. It is one of the evidencebased interventions that has been shown to work in regards to falls prevention for inpatients, so we use that on our older persons ward,’ Keith says.
The risk of falls among older patients, in particular, who are admitted to hospital are high; this patient cohort is generally unwell, they’re weaker, they may have impaired vision, some may be dizzy and those who are ambulatory often require assistance. Keith says data collected by the health service and utilised by the Cairns and Hinterland Falls Committee drives the interventions used to help reduce the risk of falls. The falls champions on the hospital’s wards help educate nurses about procedures and policies around falls prevention, about the equipment that can be used for mobility, about safe mobility practices and about helping to get patients up and about.
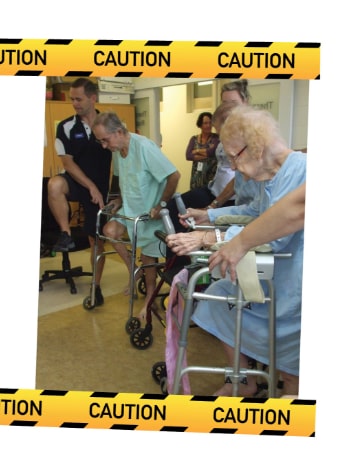
‘I suppose people might think it’s bad to have a lot of falls but there’s two sides to a fall in regard to how many injuries are occurring and with your dignity at risk for patients. Because if we tell every patient to sit down and never get up and move, we’re actually deconditioning
patients in hospital. A really important balance is making sure that patients can get up and move,’ Keith says.
‘The CHHHS has a lot of actual falls but we have a very low … number of injuries because we have a lot of what they call “assisted falls”. This means we’re responding to alarms when patients are trying to get out of bed so then we can hopefully get to them before they start to fall, or lowering them to the floor.’
Keith says to help keep up with the latest research he is part of a journal club that has members from Rockhampton, Townsville and Cairns hospitals as well as community services dial into regularly, and he plans to attend the Australia and New Zealand Falls Prevention Conference which happens every two years. This year it is scheduled to take place in Auckland, New Zealand, in November.
‘When you are talking about research, our high-risk cohort are those with cognitive impairment—and a lot of the time those patients are excluded from studies because there’s ethical reasons,’ Keith says. ‘It’s more difficult to get a study up and running when you’re including patients with a cognitive impairment. So when you’re looking at the research you need to consider which cohort’s been included in that study because there’s very few that actually has looked at your cognitive impairment group.
‘From my perspective, that’s our highest risk cohort in an inpatient setting. Those patients who have a delirium postop or they have a dementia and, again, in an unfamiliar environment there can be triggers for behavioural and psychological symptoms of dementia that can be difficult for the patient. So it’s really important to know what is the best routine and pattern and what works with those patients when they’re in an unfamiliar environment in hospital.
‘From a falls perspective, it’s everyone’s business in the hospital to work on falls prevention. You shouldn’t rely on the nurse on your ward or your physio—it’s a team approach. From a hospital setting, it’s a collaborative approach to achieve the best outcome, which is hopefully no falls but, realistically, it’s about minimising harm and minimising the incidence of falls, because they will occur.’
A multi-systems approach to falls prevention in hospitals requires good organisational strategies along with good clinical strategies, says Curtin University researcher and APA Gerontology Physiotherapist Professor Anne-Marie Hill. As part of a team, Anne-Marie has led three large trials and several smaller trials based around a central tenent of physiotherapists providing patient education to older people about how to prevent themselves from falling in hospital.
`Physios are a really key part of falls prevention. One of the strongest pieces of evidence we have is that falls occur when there’s a mismatch between the person attempting to do a task or their mobility, and their actual ability. They may attempt to do something in hospital and they don’t have safe mobility, so physios being involved in assessing patients’ mobility and providing good instructions to patients and staff is really important.’
She says part of the whole-of-systems approach in the hospital setting is to ensure the environment is safe, that patients have access to the correct mobility aids, that call bells are within reach, that there is good reporting and feedback between hospital staff and that there are systems in place for recognising a patient’s individual risk factors. Underpinning that is the need for patient education around falls prevention.

‘There are some patients who may be unwell and confused and are unable to take on education, but for patients who can understand it’s really critical because we know—and we have our own data on this from our clinical trials—that over three-quarters of all people fall when they are by themselves. So this means that we need to give people education because it’s decisions they make when they’re not with a staff member that lead to them falling.
'Education is really, I think, as a researcher, one of our most promising areas to explore.’
Residential
A fall can often be the reason an older, previously independent person might make the transition from their home to residential care, or from their residential care home to a higher-care facility. And it is at this point that physiotherapist Amy Hill, APAM, meets many of her clients. In her role working in residential aged care in Sydney, Amy works specifically with patients who have dementia. This population is very high-risk of presenting to hospital after a fall, many with hip injuries.
‘The way I look at it, is that I do work with people in their own homes. Even though I am in a residential service, it is their home, it’s not like a hospital so I still have the same philosophy in the way that I work in that setting,’ Amy says. ‘I find that I really enjoy this type of work, going into someone’s home and being guided by them. It’s quite humbling.
‘A high number of people presenting to emergency departments with various injuries including hip fractures have dementia and are from residential care. Falls are catastrophic for this population. Not only do they need a hospital admission but they also need pain care, and the fall is often the catalyst for an enormous change in their life.’
Amy says one of her passions is to stop falls from happening in this patient cohort. It has been suggested that more than 60 per cent of residents of aged care have a fall each year, and that falls are the leading cause of preventable deaths in residential aged care.
‘Although we can’t undo dementia—it is a progressive disease—if we can make that journey kinder, smoother, less crisis-driven and more of the gradual, supported decline, it’s much better for the person with dementia and for the family around them,’ Amy says.

‘What we do know is that falls are multifactorial, and research is coming out about the cognitive component of mobility and balance. There is certainly a link between cognition and how well you can walk. One of the things researchers are finding in dementia research is that changes in gait pattern might be some of the first signs that someone might have a cognitive impairment. So, there’s probably a link there.
‘Also an increase in falls risk for the person living with dementia may be related to impulsive behaviour or less insight into risk. The person with dementia might not totally understand that they don’t have the balance on board, that they’re not judging the situation as well, and that a fall can happen. The third thing is that with falls prevention measures, the person with dementia might not be able to cognitively adopt them. The person living with dementia may choose their slippers purely on comfort. Whereas the person without dementia might say “I like them but they’re not very safe.”.’
Before working in community services and then on to the residential care sector, Amy spent two years working under a different funding model of care for the older population in the UK.
‘In the UK, I worked for an intermediate care service, which was community based. I was able to support older people at home. We could do a lot with hospital avoidance. We worked really closely with the acute hospitals making sure that there weren’t unnecessary hospital admissions. It was a really lovely and rewarding job.
‘However in Australia, the biggest challenge—and the saddest thing—is that there is no direct funding for a physiotherapist to do falls prevention in residential care. There is an expectation by the government, through aged care standards, that say we should be doing it, but because of ACFI [the Aged Care Funding Instrument] there is no direct funding via that for falls.’
Amy says the funding provided by the government is geared towards pain management. Interventions such as exercise, which are also good for pain management, are not funded. ‘If we had a better aligned funding instrument with the standards and with evidence-based practice, it would be great because the interventions we use for pain would also help with falls. But right now, we’re trying to, on a very skeleton service, prevent falls and manage pain and meet funding requirements—and it’s really difficult.’
The APA has been lobbying for change in this arena (see article below) and Amy says that as part of her role on the APA’s New South Wales branch council she wants to help better connect the acute, community care and residential care sectors. ‘Our work affects each other so strongly, and I think there’s a lot more we can all work on together. We want to be able to show the government that we’ve all got the same sort of plans, although coming at it from different angles, but that we are working towards the same goal—improving the services for older people.’
One of the difficulties in the residential care setting is that there is limited evidence about what works, says Professor Anne-Marie Hill. ‘We know that falls in a residential care setting are one of the greatest concerns we have and that is mentioned in the latest Australian Institute of Health and Welfare data too. Through reasonably large systematic reviews, it is now suggested that a good basis is to use multifactorial strategies in the residential care setting, just as they do in hospitals.’
This is through the three key areas of having individualised falls risk management of patients, provisions of a safe environment and that organisations have good training, practice and communication in place.
‘The strongest evidence we have, and one of the most powerful things we look at, is that people who live in nursing homes should be receiving vitamin D supplementation because that is known to reduce the rate of falls. Vitamin D supplementation for frail older people is especially goodas these older people are at high risk of falls.
‘We’ve got very strong evidence that exercise is what you should do in the community to reduce your risk of falls— and that’s very strong established evidence,’ Anne-Marie says. ‘But until recently it’s been a little bit mixed in nursing homes as to whether that would work. There’s been a recent trial [The Sunbeam Trial, see separate article on this website], which was done in a population of people who live in nursing homes, about whether exercise reduced falls. That, I think, shows that exercise is important in nursing homes for older people who can participate in it, because obviously some of these people can’t.’

The theme for April Falls Week 2020 is ‘Stay safe— communicate’ to encourage communication of patient safety risks between healthcare workers and their patients, families and carers. It is hoped the open dialogue will promote falls risks as well as make falls everyone’s business, themes being promoted by the NSW Falls Prevention Network during this month’s activities.
The planned NSW Falls Prevention Forum, which was to be held in Sydney next month, was cancelled due to the coronavirus. However, the forum plenary talks will be presented in a free webinar on the morning of Friday, 15 May. Registration is essential on the NSW Falls Prevention Network website (tinyurl.com/wgken9c). To find out more about April Falls Week visit fallsnetwork.neura.edu.au.
Advocating for change in the aged care sector
The APA has been an active participant in the reshaping of the aged sector with substantial advocacy calling for improved funding for preventive, restorative and reablement care and improved access to physiotherapy for older Australians.
The Royal Commission is providing multiple opportunities to put forward the physiotherapy perspective. The timelines provided are very tight and the workload demanding.
The APA is working closely with Board Director Rik Dawson, National Gerontology Chair Vanessa Jessup, the national gerontology advisory committee, researchers Katherine Lawlor, Dr Jennifer Hewitt and Professor Anne-Marie Hill to develop submissions.
We are using every opportunity to:
- raise awareness of the benefits of physiotherapy for older Australians
- seek early assessment by allied health professionals of older Australians entering the aged care system
- introduce dedicated funding for physiotherapy restorative and reablement care
- encourage funding for research
- seek establishment of an aged care steering committee to develop research into best practice workforce models.
The APA has made five submissions to the Royal Commission into Aged Care Quality and Safety since January on:
- a general response to the inquiry
- workforce
- program redesign
- dementia, ageing and aged care (research)
- response to workforce recommendations.
We expect to contribute further submissions in the coming months. The APA has also participated in two Primary Health Care roundtables on dementia and older people.
We are working with the National Aged Care Alliance, Australian Health Professions Australia, individual associations and others to ensure the profession is represented at upcoming workshops on reshaping the aged care sector.
To find out more about the APA’s advocacy work visit australian.physio/advocacy.
Taking steps to stay on your feet
Simple steps that patients need to consider to avoid taking a tumble while they’re in hospital are detailed in the Be Safe brochure, produced by the ‘Stay on your Feet’ falls prevention program.
The brochure, distributed in hospitals nation-wide, details general principles that patients can follow including looking at the suitability of their footwear as well as offering valuable advice on hazards, medications and how to best access safety equipment.
The Stay on your Feet website includes a portal for practitioners to access and includes social media tiles and printable posters, brochures and fact sheets to download, as well as links to eLearning and an eDirectory to locate falls prevention classes and activities across the state. There is also a section for the latest news in falls prevention and a portal dedicated to helping people in their 60s.
The ‘Stay on your Feet’ evidence-informed programs promote strategies for older adults to reduce their falls risk so that they can stay active and independent for longer. The messages are targeted at health professionals as well as older adults who live in the community, their family, friends and carers.
To access the ‘Stay on your Feet’ tools, visit stayonyourfeet.com.au.
© Copyright 2024 by Australian Physiotherapy Association. All rights reserved.





