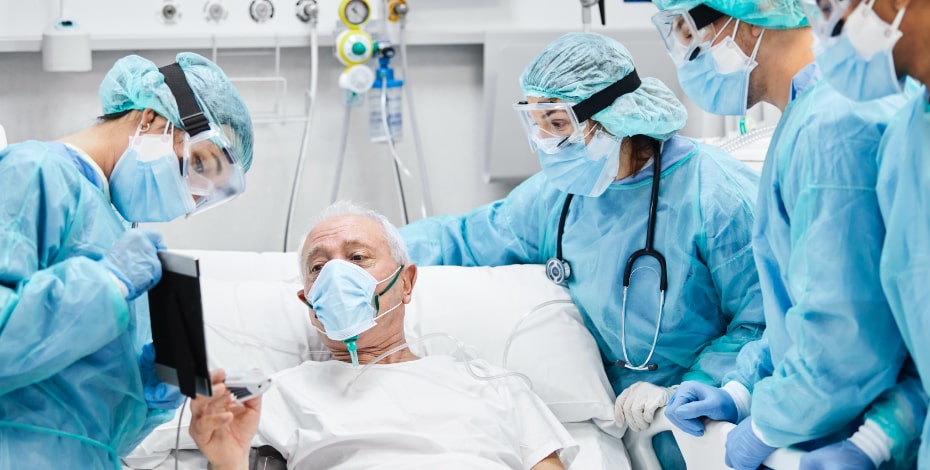
Caring for older adults in a pandemic

Physiotherapists play an important role in Australia’s response to the COVID-19 pandemic, including the care of older Australians needing rehabilitation during inpatient stays. Meeting this need poses unique challenges, requiring innovative thinking from ward-based physiotherapists.
As Victorians face another lockdown in June this year, Jacqui Kay, Jessica Huglin and Taree Gibson share their insights and discuss how working on the frontline affects the practitioner and the person.
What was your role and what were your main duties during the pandemic?
Jacqui: I am the clinical lead physiotherapist for aged care at the Royal Melbourne Hospital’s (RMH) Subacute Campus.
During the pandemic, I led the planning for the subacute site including the development of the RMH COVID-19 clinical practice guidelines for subacute physiotherapy, which involved a significant shift in treatment of patients on the wards.
I also led work around staff planning to ensure risk mitigation and wellbeing was maintained as much as we could control.
I worked clinically on the COVID-19 ‘hot’ wards at the subacute site during the outbreak we had.
Jessica: During 2020 I worked as a general medicine physiotherapist as part of Monash Health’s Acute and Complex Care team at Dandenong Hospital.
During the pandemic response I provided physiotherapy services to acute inpatients with confirmed COVID-19 and suspected COVID-19 (SCOVID).
My main duties encompassed referral management, transfer and mobility assessments, exercise program prescriptions, education provision, equipment management, respiratory care, discharge planning and follow up referral management.

Jacqui Kay
Additionally, I was the allied health leader for our SCOVID ward.
During a period of personal furlough I provided remote support to colleagues onsite to manage referrals, screen new patients and work on the ward when required.
Taree: I worked as the Allied Health Manager and physiotherapist on Holmesglen Private Hospital’s COVID-19 ward during our public pandemic contract.
My main role was providing cardiorespiratory treatments, mobility reviews and rehabilitation for baseline comorbidities or secondary acquired impairments.
What is your strongest memory from that time?
Jacqui: A very strong memory is a patient who had been admitted to the ward with COVID-19 from an aged care facility. She was a wanderer and was very confused. She would often follow me around the ward asking, ‘Why am I here?’ and ‘When can I go home?’
It was the only sense of normality I could find during a very stressful time, as this is what patients on that ward did before we had ever heard of COVID-19.
Among the fear, anxiety and being in flight/fight mode for so long, this patient was someone I looked forward to seeing every day.
Jessica: How much longer everything took. In minimising potential exposure time, referrals were remotely screened with the nursing staff and the extra phone calls to patients and families when you couldn’t just ‘duck back up to the ward’.
Additionally, the extra infection preventing processes such as getting changed into and out of scrubs, the PPE donning and doffing processes. It all seemed to add up very quickly.
Taree: The smell of shampoo, as I washed my hair after every shift. And I recall the feeling of unity and purpose among the multidisciplinary team working on the COVID-19 ward. There was a sense of quiet pride in what we were doing.
What were the major challenges you faced working with COVID-19 positive older adults?
Jacqui: The biggest challenge was that our expectations of providing rehabilitation post-acute COVID-19 infection did not meet the reality of dealing with an acute outbreak at the subacute site.
Physical rehabilitation was challenging due to the severity of symptoms patients were experiencing on the ward and the speed of deterioration.
Our usual tricks to motivate patients to exercise were also removed—we were unable to run groups, take patients outside or get family members involved.
We also found it very difficult to build rapport with patients due to the amount of PPE that was required to work on the ward.
Jessica: One of the main challenges was logistics. The basic practicalities of getting to the ward in the right attire with the right patients to see, setting up the right equipment and ensuring you didn’t need to double back for anything.

Jessica Huglin
It all required pre-thought and planning with the nurses on the ward.
Secondly, and more specifically to older adults, the sheer ‘newness’ of what we were dealing with. At the time there was more of a spotlight on the ICU management of these patients than on supporting their early rehabilitation, either post an ICU admission or not.
The complexities of discharging patients home, often to complex social situations related to the COVID-19 outbreaks in Victoria, was challenging and required creative thinking, especially in the older adult population.
The benefit at Monash Health was that we had two other COVID-19 positive general medicine wards to collaborate with as a clinical team.
How did you manage to facilitate rehabilitation for COVID-19 positive older adults?
Jacqui: We literally did the best we could with what we were presented with. Symptoms (predominantly fatigue) were really big factors on rehabilitation, both in the acute and subacute stages.
We offered therapy to those who could participate, for short, sharp bursts multiple times per day rather than long sessions. The focus was on strengthening, pacing and mobility progression, all while monitoring exertion.
Jessica: As physiotherapists we are often motivating our acutely unwell patients and encouraging them to partake in activities on the ward. COVID-19 and the related symptomology—specifically reduced appetite and oral intake—made patient participation very challenging.
There was often a lot of education and encouragement to family, nursing and medical colleagues as to the importance of early rehabilitation.
Facilitating rehabilitation required careful planning including timing of entering the ward, having nursing staff around, and finding out what motivated the patient and what their goals were.
We had an older couple, both from an aged care facility, who were motivated to do things related to being visible to each other, so any kind of activity related to seeing each other was often well received.
Taree: We had one patient develop an acute stroke as a secondary impairment. Options were explored regarding acute stroke rehabilitation for them, but because everything was so dynamic, we had difficulties transferring them to a dedicated unit.
So in the meantime, we began their rehabilitation on the ward, within the resource constraints we had.
Nurses and personal care assistants became therapy assistants for facilitation, acute swallow assessments happened over FaceTime, and the patient needed to do a lot more self-directed practice than traditional service delivery.
What were some of the facilitators or things that worked well?
Jacqui: We tried to have consistent therapists who would work on wards for two weeks at a time.
We had a ‘buddy’ system for donning and doffing PPE for safety, and we often would co-treat with other physiotherapists and allied health assistants to ensure we were maximising each session with patients.
We would try to time sessions around their care needs and also complete sessions for short periods because they would tolerate it.
Jessica: Keeping in the loop with the rest of the multidisciplinary team was key. In my role I was sometimes the ‘eyes and ears’ on the ground.
For example, being aware that the dietician was trying a new supplement with a patient because of a flavour preference meant I could be on the lookout for the signs that the patient was improving and might be more likely to participate in rehabilitation.
Working efficiently within our multidisciplinary team also meant optimising our interactions with the patients to reduce patient fatigue on things such as phone and video calls. The end result was that the team was across everyone’s discharge plan.
Lastly, we were phenomenally lucky to have such a fabulous nursing team with the patients around the clock, with a direct line to ask about how the patients were going with their activities on the ward.
In the unit we had staffing to be able to work with the nurses on what activities the patients could do during the day, whether that be rehabilitation (strength exercises) or respiratory-based (weaning recommendations, spontaneous prone positioning regimes).
Taree: A clear communication pathway with the team. We set up a morning meeting so that the nurse unit manager could update the allied health team on patient status.
Then the therapists could respond to referrals, online as a first pass or face-to- face as required. Being able to supervise the nursing staff via video in order to reduce transmission risk by having fewer therapy staff on the ward also helped.
What would be your biggest learnings to share with physiotherapists around the world working with COVID-19 positive older adults?
Jacqui: My advice would be to look after your staff and each other. The safety and wellbeing of staff is paramount to the success of a department during a pandemic.
The need to work as a team and for each other, not just in the physiotherapy department, but also with your allied health, nursing and medical colleagues, is never more important.
You are all in it together and the better you work together, the safer the situation can be, with the best outcomes possible. I would encourage staff to seek support for their mental health through avenues offered within and outside their organisations.
Jessica: In particular for the older adult, the biggest learning for me was around how a person’s pre-existing health state, social situation and medical history were impacted by COVID-19.
This often led to more consideration about chronic condition management in the unique physical set-up of the ward (eg, delirium management) and the huge impact that reduced oral intake can have on the older adult.
Education and strategies to implement any physiotherapy or allied health recommendations needed to be tailored depending on the individual’s cognitive state, and discharge planning had multiple layers of complexities when considering those older adults who require physical assistance in their everyday lives either at home with family/carers or within supported accommodation/aged care facilities.

Taree Gibson
The complexities of COVID-19 for the older adult cannot be overstated and I really look forward to the continued shared learning as a discipline.
Taree: Being aware of the best practice guidelines being released by local and international peak bodies. The APA Cardiorespiratory guidelines for COVID-19 adults were paramount in knowing how to respond to the patients we were working with.
It’s important to have excellent lines of communication between the multidisciplinary team to allow for good handover, alignment of goals and supervision of staff performing non-traditional scope of practice tasks (eg, the personal acre assistant performing exercise for a patient under the supervision of the physio, in order to reduce transmission risk between patient rooms).
Can you share your reflections on what impact this experience has had on you as a clinician or as a person?
Jacqui: This experience has reinforced for me just how amazing and resilient healthcare workers are.
We are the frontline workers who continued to show up every day, even though we were putting our health at risk by doing so. In the words of Winston Churchill, ‘never waste a good crisis’, and we didn’t.
The team I worked with were still able to achieve really great things and have significant impacts on our patients’ lives in a time of crisis in Melbourne.
Jessica: It was, as for so many, a very challenging year. With changing work environments, clinical roles, periods of furlough at home in quarantine and uncertainty in our COVID-19 admission numbers, there was always something to process with what were sometimes highly emotional situations for the multidisciplinary team.
Although not something we ever wanted to happen, this experience was something I was glad I could play a role in for my own clinical development. To be a leader and support person for my team was rewarding.
There remain some parts of the whole experience that still don’t seem quite real (14 days of lockdown in your own home seems fun until you hit day 3).
However, like many healthcare workers I am sure, I felt proud to know that I was doing something to help those who were acutely unwell with COVID-19
Taree: Working with COVID-19 positive older adults has been the highlight of my career, something to tell the grandchildren about. I would go back and do it all again, although I hope we never have to.
That being said, it is important to acknowledge the mental health burnout that healthcare workers are experiencing even now, in 2021. I would encourage my colleagues to reach out to your local GP and discuss this with a professional if you are still feeling the effects of a very difficult 2020.
Jacqui Kay is the Grade 4 Clinical Lead physiotherapist for aged care at the Royal Melbourne Hospital subacute campus. Jacqui has a passion for physiotherapy management of chronic diseases and vulnerable populations as well as positive team culture among physiotherapists. She has worked extensively in these fields in Australia and the United Kingdom.
Jessica Huglin is a clinical physiotherapist working at Monash Health’s Dandenong Hospital. There, she is part of the Acute and Complex Care stream, providing inpatient physiotherapy services to patients across the Emergency Department (ED) and General Medicine wards. Jessica has a clinical interest in the complex discharge planning of the older person from ED and a passion for data based quality improvement activities.
Taree Gibson is an APA Gerontology Physiotherapist and has a master’s degree in rehabilitation (gerontological physiotherapy). Taree has 10 years’ experience working with older adults.She is passionate about advocacy for the older adult and learning from her patients, is motivated by collaboration and enjoys sharing knowledge and experience with colleagues.
From clinical to strategic care, core physio skills still count
Sarah Miller is proof that a physiotherapist’s skills are transferable. As Marina Williams writes, Sarah has tackled COVID-19 from both within and beyond the four walls of the hospital, in clinical and community settings. And her work, it seems, is not yet finished given June’s circuit-breaker lockdown in Victoria.
More than 18 months into a fast-moving coronavirus pandemic, Sarah Miller’s transferable skills ensure that the physiotherapist and transdisciplinary therapist remains a vital part of the national response to COVID-19.
Key to her past and current roles is restoring some sense of normality in communities as the pandemic continues to unfold.
Sarah was first introduced to COVID-19 when working at one of the UK’s largest medical facilities, Kings College Hospital NHS Trust, in early 2020.
With her solid respiratory skills, the clinical physiotherapist quickly became responsible as team lead for physiotherapy management of patients stricken with the coronavirus.
She was involved with decision-making on access to intensive care, leading a prone team, making life support recommendations and starting early rehabilitation.
On arriving home, Sarah continued in clinical care on the suspected COVID-19 ward at The Alfred in Melbourne.
Then, as Australia shifted into a stage of recovery and community transition, she moved from frontline support to readiness response with the Human Services COVID Readiness and Response Centre (HSCRRC), formally known as Operation Benessere.
The taskforce was established in Victoria in mid- 2020 after the public housing lockdown and provided ongoing prevention, preparedness and rapid response in high- risk shared accommodation facilities. It was her fifth COVID-19 job in a year across London and Melbourne.
HSCRRC has since been integrated into the Department of Families, Fairness and Housing for ongoing proactive readiness and response work to prevent the spread of COVID in high-risk settings within the Victorian community.
‘I understood what it is like for people needing and experiencing care in a clinical setting and those most at risk of severe illness. Skills I learnt clinically, like risk analysis, helped me to solve problems laterally and provide collaborative leadership.
'Working in three hospitals in two countries during COVID-19, I have seen the difference between having a healthcare system that was prepared and one that was not.’
Sarah was one of many specialists on the taskforce, combining her clinical, analytical, project-planning and emergency- management skills to provide coronavirus-related assistance to the housing sector that included government and non-government-run specialist residential services and rooming houses.
Having public health measures in place in public housing and other high-risk accommodation settings remains vital to preventing virus outbreaks and mitigating its impact, Sarah says.
With much of her clinical career in emergency departments, as well as being a long-time volunteer and a former president of St Vincent de Paul Society Soup Van, she understands the importance of including vulnerable communities in health decisions.
‘Each individual person and their own needs are important when making impactful health decisions. A global pandemic that is contiguous and emergent knows no borders.’
For six months at HSCRRC, Sarah honed her operational and stakeholder engagement skills as the safety lead between health providers and community groups. Her team was responsible for ensuring that the COVID-19 safety principles of test, trace and isolate could be met.
‘This was particularly important during the rollout of COVID-safe plans statewide,’ she says. ‘The focus of the response shifted towards preventing, preparing for and responding early to COVID-19 infection, to minimise transmission in accommodation settings.’
Sarah says years working in clinical environments in hospitals and various leadership roles has provided a good foundation for her most recent shift into a more strategic role for management during the ongoing pandemic.
In March, her experience in systems thinking within the health sector saw her become senior strategy advisor for the Deputy Commander of Operations at COVID-19 Quarantine Victoria (CQV).
CQV was formed in November 2020 as part of the state government’s response to the COVID-19 Hotel Quarantine Enquiry’s interim report. It oversees all parts of the Victorian quarantine program.
The agency underwent a review in late February when the state’s hotel quarantine program was paused after COVID-19 community transmission, prompting Victoria to put in place a snap five-day lockdown earlier in the month.
With a revision of rules and regulations in the program, international flights to Melbourne resumed in early April.
Sarah joined during the review and is contracted until November. Her role is primarily one of driving best practice in program delivery.
In balancing the day’s urgent priorities and thinking forward to provide more strategic decisions, she liaises with agency groups, such as border force police, interstate jurisdictions and frontline staff on the ground.
She says her physiotherapist skills and global experience have been central to moving from frontline response to strategic leadership in responding to the global pandemic.
‘One of our most basic physio skills is our clinical “SOAP” notes—we listen, we measure, we analyse and then clearly, concisely communicate with all walks of life.
'All day, we are talking to all members of our wider team of health professionals and families, about a better way to help our patients and deliver care,’ Sarah says.
‘As a hospital-trained physiotherapist, you also have a good understanding of governance and an ability to analyse risks and communicate when needed, as well as understanding complexity in an environment like this, including the technical understanding of infection control and emergency management, but also the leadership required with the number of interdependencies that can occur.’
© Copyright 2024 by Australian Physiotherapy Association. All rights reserved.






