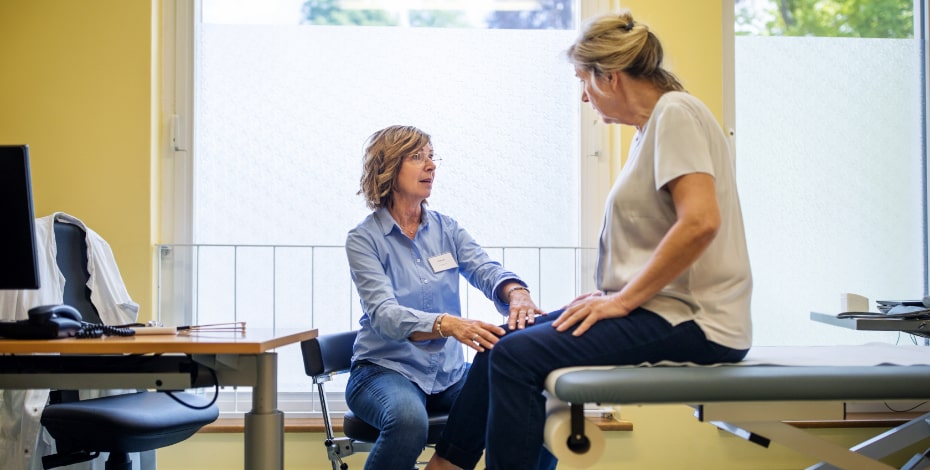
Physiotherapy care for knee osteoarthritis

What are the experiences of physiotherapists delivering care for people with knee osteoarthritis, and how do these experiences align with the national Clinical Care Standard? Q&A with Rana Hinman and Samantha Teo.
Professor Roberta Shepherd is an APA Honoured Member and an Honorary Professor at Sydney University. She is a pioneer in neurological and paediatric physiotherapy, working throughout her career as an educator and researcher.
Roberta has published many textbooks in collaboration with Professor Janet Carr (deceased) on topics including stroke rehabilitation, movement science and cerebral palsy.
Your recent survey sought to gauge whether Australian physiotherapists’ management of knee osteoarthritis was aligned with the Australian Commission on Safety and Quality in Health Care’s ‘Osteoarthritis of the Knee Clinical Care Standard’. What is the purpose of the Standard?
The Standard is a set of nationally agreed quality statements that describe key aspects of care that should be offered to patients with knee osteoarthritis (OA). The Standard was established to support clinicians to deliver evidence-based care to people with knee OA and to minimise variations in care.
Did you have a broad range of physiotherapists involved in the study?
Yes, we included a range of physiotherapists from across Australia in our interviews.
We interviewed 22 physiotherapists ranging in age from 24 to 54 years. More than three-quarters (77%) worked primarily in private practice.
Physiotherapists were from Victoria, New South Wales, Western Australia, Queensland, Northern Territory, South Australia, and the Australian Capital Territory. Physiotherapists spanned major cities, inner regional, outer regional and remote areas of Australia.
What aspects of physiotherapists’ management of knee OA was aligned with the Standard?
Physiotherapists’ care generally aligned with most domains of care described in the Standard. The first domain of care relates to comprehensive assessment.
Physiotherapists generally conducted a comprehensive subjective and physical examination for the knee. They recognised the importance of evaluating a patient’s overall functional ability to determine functional goals.
The second domain of care focuses on diagnosis. Physiotherapists tended to diagnose knee OA clinically and used imaging to rule out serious pathology, but sometimes also used it to confirm a diagnosis.
The third domain of care concerns OA education and self-management.
Physiotherapists generally informed patients about what knee OA is and discussed self-management strategies that were mostly aimed at addressing biomechanical aspects of knee OA.
The fourth domain of care focuses on weight loss and exercise. Exercise was the central management strategy utilised by physiotherapists for knee OA.
Physiotherapists favoured a tailored exercise approach that considered individual preferences, physical ability, personal needs, affordability and/or accessibility to exercise facilities, and established personalised exercise goals with patients.
Physiotherapists tended to advise patients who were overweight or had obesity about the importance of weight loss for knee OA and sometimes referred patients who needed to lose weight to other healthcare professionals (eg, GP, dietitian etc.).
The sixth domain of care relates to patient review. Physiotherapists typically offered regular reviews to patients with knee OA.
Were there any aspects of care where physiotherapists could offer more?
The two domains of care where physiotherapists could offer more to their patients with knee OA concern medication (domain five) and surgical advice (domain seven).
Physiotherapists could be more proactive in offering information about the potential benefits and harms of common knee OA medications and surgical treatments so that patients are fully informed about their treatment options and can more actively participate in shared decision-making.
Physiotherapists’ assessment of the patient could benefit from a more holistic approach that considers relevant psychosocial factors that may influence OA symptoms and prognosis.
Education about OA and self-management strategies could be broadened from a predominant biomechanical focus to incorporate psychosocial contributors to the pain experience.
In addition, given the greater workforce capacity of physiotherapists in Australia relative to dietitians, physiotherapists could consider providing more information to patients about potential strategies for weight management.
Finally, physiotherapists could also consider offering more regular reviews over the longer term to monitor patient symptoms and to ensure timely intervention and/or referral is provided if required.
And are there services currently being offered that should be curtailed?
Physiotherapists often relied on imaging to ‘confirm’ a clinical OA diagnosis; however, clinical practice guidelines advocate for a clinical diagnosis of knee OA without the need for imaging.
Unnecessary imaging may reinforce negative patient beliefs about OA, reduce patient engagement with lifestyle management strategies such as exercise and weight loss, and is costly to the health system.
Physiotherapists should also be judicious about their use of adjunctive manual therapy to ensure that it is not used at the expense of the core recommended knee OA treatment strategies of exercise, education, self- management, and weight loss (for those who need it).
This seems reassuring for both patients and the profession. Do you agree?
Yes, physiotherapists are important providers of care for people with knee OA.
They have a pivotal role to play in providing core treatments for knee OA, including exercise, weight loss, and education about self-management. Provision of a high-quality evidence-based care to patients with knee OA is integral in the effort to achieve better patient outcomes.
What about future research in this area?
Future research could focus on developing, implementing, and evaluating strategies to better support physiotherapists to provide more comprehensive advice and information to patients, that incorporates psychosocial issues, weight management strategies, and information about medication and surgical treatment.
Click here to access the papers featured here, and others, from the latest issue of the Journal Of Physiotherapy.
Professor Rana Hinman is a physiotherapist and NHMRC Senior Research Fellow at the Centre for Health, Exercise and Sports Medicine at the University of Melbourne. Her research focuses on clinical trials of non-drug, non-surgical treatment strategies for osteoarthritis, in particular exercise, rehabilitation, and biomechanical interventions.
Samantha (Pek Ling) Teo is a physiotherapist and PhD candidate at the Centre for Health, Exercise and Sports Medicine at the University of Melbourne. Her PhD evaluated the quality of physiotherapy care for people with hip and/or knee osteoarthritis.
© Copyright 2024 by Australian Physiotherapy Association. All rights reserved.





