
Taking the travel out of stroke recovery

A pilot project underway in Western Australia is having a huge impact on helping acute stroke patients stay close to home in their rural community. Melissa Mitchell reports.
A terrible headache unlike anything she had ever experienced sent Janet Cozens early to bed one night in June last year. The evening news had just come on television but Janet took herself to bed to sleep off the blinding pain, which she says made her feel as though her left eye was going to burst. Her husband, David, checked in on her throughout the evening and believed Janet was sound asleep. When David decided to retire for the night, he woke Janet to check on her but it quickly became evident that something was very wrong.
‘When he woke me I told David “I’m going to go to the toilet” and I stood up but I fell right back on the bed again, my legs didn’t have any strength in them whatsoever,’ Janet says, talking to InMotion from her home in Geraldton, 424 kilometres north of Perth, Western Australia. ‘My husband managed to get me to the toilet but I was a dead weight, my right side wasn’t working and the right side of my face had dropped.’
Janet had atrial fibrillation and had suffered an embolic stroke that had severely impacted her right side. An ambulance was called to rush her to nearby Geraldton Hospital, where she was to spend the next four weeks. Unable to walk or use her arm, Janet was introduced to the physiotherapy team and her therapy began. As soon as she was able, Janet was treated on the ward twice a day for rehabilitation, and key to that was the incorporation of telehealth in her recovery plan.
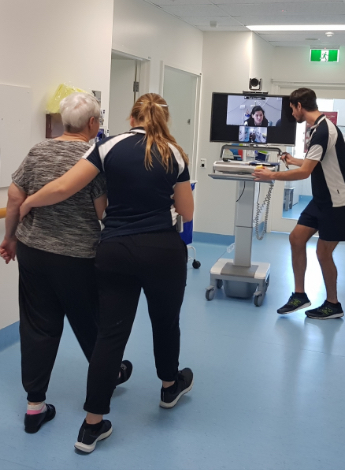
As part of the Western Australian Country Health Service (WACHS) and North Metropolitan Health Service (NMHS) TeleStroke- Rehabilitation pilot project, physiotherapists at Geraldton Hospital can link up with Jessica Nolan, APAM, the physiotherapy coordinator of stroke and in-patient rehabilitation at Osborne Park Hospital in Perth’s north-west, via video link using a telecart. The portable videoconferencing unit brings the Geraldton physiotherapy team and their stroke patient together with Jessica for rehabilitation sessions. Jessica also attends weekly multidisciplinary team meetings via telehealth, when the Geraldton team meets to discuss their stroke patients.
Before the pilot project began in April 2018, Jessica and a team of occupational therapists and consultants travelled from Perth to meet the Geraldton team in person. ‘I think that [face-to-face meeting] made a huge difference because we got to know and trust each other better. We also got an understanding of their services and facilities onsite. I think getting to know each other makes the difference … when you don’t really know someone but you’re giving them advice and instructions you can feel a bit awkward, so it is better to develop a relationship with the team,’ Jessica says.
When she first joined the pilot project, Jessica thought her involvement would be limited and that the service would perhaps be better suited to occupational therapists and other allied health disciplines. However, she quickly realised the practical implications for physiotherapy were great, although it required her to rethink some of her practices, including training herself to explain interventions rather than showing with her hands how to perform them.
‘I was nervous at first because in stroke rehab I’m so used to being able to touch the patients. I do interact with patients via telehealth as well, and give instructions and explanations to them, but it’s more of a coaching and mentorship role with the clinicians in Geraldton,’ Jessica says. ‘I have had to get a lot better at explaining things; I’ve had to sit on my hands and figure out how to explain it, which has been quite good for me. From a physio point of view, telehealth is a really fun thing to do and you challenge yourself with getting to know different patients and understanding different services and some of the challenges in rural areas.’
Jessica says her role has been one of mentoring and advising on patient gait mobility and manual handling as well as offering support and advice to physiotherapists in Geraldton, including Liza Doble, the senior physiotherapist on the inpatient ward. Liza, who is involved with acute and subacute rehabilitation, says although telehealth is common in rural settings, being able to use the mobile telecart and having senior support available from Perth has worked really well at Geraldton.
‘Before I came to Geraldton I worked on a rehab ward so I’ve had some experience with stroke. But after being here for four years you become quite a generalist physio so I feel like it’s a huge support for me to have Jess’s knowledge and expertise available,’ Liza says. ‘It’s great having the senior support from Perth, the specialists in stroke. They’re all up-to-date with the latest evidence so you know your patients are getting the latest evidence-based practice.’
Since the pilot project was introduced, Geraldton Hospital has seen a significant reduction in the number of stroke patients needing to travel to Perth for rehabilitation treatment, which increases rural self-sufficiency. WACHS telerehabilitation project manager Ruth Warr, who is based at Geraldton Hospital, says about 92 per cent of patients presenting to Geraldton Hospital after stroke have been able to stay in Geraldton as of 30 June this year. To give that some context, in 2016/17 more than 30 per cent of stroke patients were transferred to Perth for specialist stroke rehabilitation. And patients being able to stay in Geraldton means less time in hospital, less disruption to families and carers, and better access to outpatient services.
The pilot project was initially funded until 30 June this year; however, the project partnership between WAHCS and NMHS has been extended until 30 June, 2020. The project has been evaluated and monitored throughout its operation, examining not only patient admissions and length of stay but also cost-effectiveness, patient and staff experiences.
‘We’ve been looking at it in terms of Midwest staff’s reaction to the service and experiences, and they are telling us that they feel a lot more confident in providing stroke rehabilitation throughout the project period. We know that regional staff are specialist generalists; that’s what they do, they deal with everything that walks through the door,’ Ruth says. ‘And stroke is just one part of that. So to be able to have some specialist support in providing a high-quality service for those patients is invaluable for an area like Geraldton.’
For stroke patient Janet—one of 25 primarily stroke and traumatic brain injury patients to be part of the project so far—she says she was able to be up and walking, aided and very slowly, three weeks after her stroke. After being discharged from hospital, Janet attended twice weekly outpatient sessions where she would walk the hospital corridors with the telecart camera on so that Jessica could observe her gait and mobility from Perth. ‘It was very easy, it was a long corridor and they would have me walk so far, then turn around and walk back again,’ Janet says. ‘Having somebody in Perth in rehab, well it just confirmed what the physiotherapists in Geraldton were doing and saying. It was really good to get that confirmation.’
Although she says she continues to have some trouble with her balance, Janet’s mobility has drastically improved since her stroke. Her husband has set up exercise equipment for her in their home and she regularly uses exercise bands, walks on the treadmill and cycles on the exercise bike in addition to completing the exercises prescribed to her by the physiotherapy team. ‘I really cannot thank all the staff enough for what they have done for me, I could not have been better treated or better cared for,’ she says.
© Copyright 2025 by Australian Physiotherapy Association. All rights reserved.





