Talking point

A systematic review on Bobath therapy and lower limb activities after stroke published in Journal of Physiotherapy late last year garnered much attention. In light of this, InMotion put some questions to Alena Scurrah, a member of the Australian Bobath Training Association.
Should you still be using the name Bobath given it has changed from the original methods?
We view the fact that the concept is evolving over time as a positive rather than a negative.
Any aspect of medicine should be continuously reviewed and refined and we should never fall into the trap of doing the same thing just because that’s the way it’s always been done.
The whole of physiotherapy is an example of this—it is very different today from what it was like in the 1950s and ’60s; however, we still call it physiotherapy.
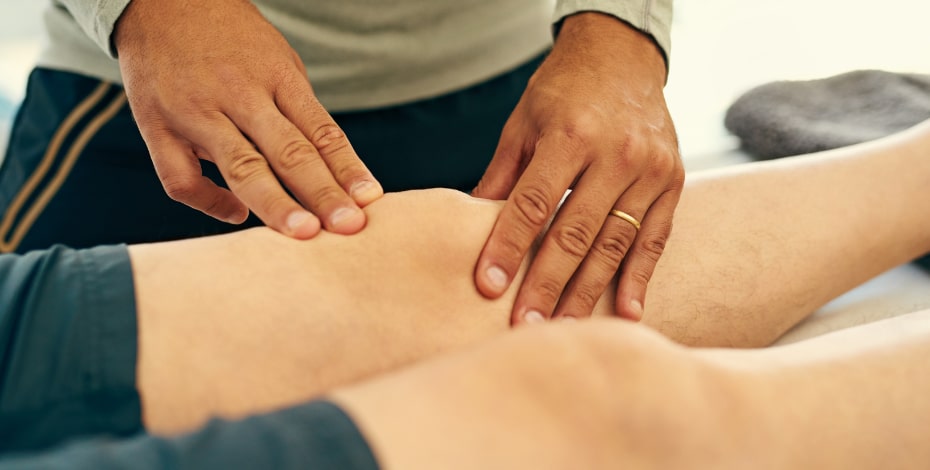
Why do you still use hands-on facilitation?
Facilitation generally, whether it be with your hands, your voice, or the way you set up the task and environment, is a staple part of rehabilitation.
Skilled facilitation enables patients to have an experience of movement that is not passive, but one they cannot yet complete independently.
A therapist is able to provide the sensory information that the patient would usually experience by influencing cutaneous receptors, proprioceptors, joint receptors and control key aspects of movement such as stability, alignment, direction, timing and range.
If all our patients got better just by giving them verbal instructions, that would be fantastic.
But we know that neurological patients often have to overcome a combination of impairments such as motor weakness, sensory dysfunction, motor planning, perceptual issues or any number of other difficulties.
As such, they are often deprived of movement experiences or compensate with disordered movement resulting in maladaptive neuroplastic changes (Jones 2017).
By experiencing facilitated movement the patient learns, and this enables the therapist to give less facilitation as the patient improves.
Nothing improves motor control more than a patient’s own movement; if they can’t do this independently, facilitation is a tool we can use to assist them.
How is clinical reasoning applied within the context of the Bobath concept?
The current evidence base, although it provides some useful information for clinicians, is seriously missing information on the clinical decision-making process.
If all our patients benefited from exactly the same interventions at the same point this would not be an issue, but we know this is not the case.
What is essential is that we understand what works, why and for whom (Tractenberg & Morris 2017).
To deliver the right interventions at the right time, therapists need to be able to analyse in detail postural alignment and complex patterns of muscle activation.
They need to understand how we control movement through multiple neurological systems. They need to be able to clinically reason their patient’s problems and how they are interlinked.
For example if a patient can’t transition from sitting to standing following a stroke, it may not be just because they have a weak hemiplegic lower limb.
They may have disordered control in their trunk preventing them positioning it in the right place at the right time of the movement sequence.
They may not be receiving or integrating adequate sensory information from their foot or lower limb and henceforth not loading the limb, and load is critical in ensuring adequate limb extensor activity (Duysens & Massaad 2015).
It may be that the patient has a perceptual or midline orientation problem causing issues with verticality or moving forward in space; there are many issues that may be making the movement difficult.
Movement problems are complex and individual. The Bobath concept provides a framework that helps clinicians problem- solve their way through the issues each patient presents with (Michaelson et al 2017).
This gives the therapist the ability to tailor the intervention to each individual rather than taking a broad brush approach, and hence increase the potential for more optimal recovery.
Is the Bobath concept a legitimate intervention in terms of the evidence base?
The Bobath concept is strongly informed by contemporary evidence from the fields of movement and neuroscience.
Unlike some other approaches, in the Bobath concept, trunk and head control is viewed as equally important as upper and lower limb control—the patient is more than just their arms and legs.
Evidence conclusively supports the importance of postural stability, and the trunk in movement control (Yiou et al 2012, Krishnan et al 2012).
Following stroke there is evidence that the degree of trunk impairment is related to how functionally impaired the patient is in terms of sit to stand (Silva et al 2015), balance (JiJimol et al 2013), and walking (Isho & Usuda 2016) and that trunk training improves sitting balance, standing balance and gait in stroke patients (Van Criekinge et al 2019).
In addition, there is now strong consensus that sensory information plays a critical role in motor control (Levin & Panturin 2011) and that we utilise this sensory information for both the feedforward and feedback control of movement (Panek et al 2014).
We also know that deficits in somatosensation affect neurological patients’ movement, balance, function and ability to learn. (Vidoni & Boyd 2009; Parsons et al 2016).
Influencing the sensory aspects of movement though facilitation has been shown to directly improve movement quality (Kogami et al 2018).
It is true, however, that more high-quality studies incorporating the Bobath concept are required, just as they continue to be required for most rehabilitation interventions.
The Bobath concept has a long history and unfortunately a lot of previous comparative studies, even contemporary ones, have used very outdated philosophies of the Bobath concept, with the intervention delivered by therapists that have had no or minimal training.
The Bobath concept is a skilled approach. Just like anything worth its salt in the therapy world, the more training and experience you have, the more effective you are likely to be at it.
The Bobath concept is taught in three-week postgraduate basic courses, and one-week advanced courses which are standardised across the world by IBITA (International Bobath Instructors Training Association).
Bobath instructors are located in 35 countries, and Bobath is one of the most commonly utilised treatment concepts around the world.
There is a reason why therapists continue to utilise the concept and continue to attend training courses and this is because they feel it greatly improves their clinical practice.
At the end of the day, every therapist is trying to do their best for their patients.
The key is having the clinical reasoning skills to ascertain what the pertinent issues are and the practical skills to address them effectively.
The Bobath concept offers clinicians both the clinical reasoning framework and the skill acquisition to do this.
It doesn’t have to be a direct choice between using different interventions. It’s about having more tools in your therapy toolkit.
All therapists who have faced the challenge of treating neurological patients know that the more options you have, the more likely you will be able to help the particular patient in front of you achieve their best potential.
>> Email inmotion@australian.physio for references.
Alena Scurrah is clinical lead physiotherapist at the Cairns Hospital Rehabilitation Unit and member of the Australian Bobath Training Association. Alena has been an Australian Bobath Tutor since 2014.
© Copyright 2024 by Australian Physiotherapy Association. All rights reserved.






