
Virtual physiotherapy: more than fun and games

Physiotherapy is, by its very nature, a hands-on form of healthcare. But new digital technologies including virtual reality and interactive video games are offering novel ways to work with clients both in the clinic and at home.
Most people think of entertainment when virtual reality (VR) and video games are mentioned.
But physiotherapists are increasingly turning to VR and related technologies to enhance their clinical practice and encourage clients to complete their exercise programs.
What is VR?
As a concept, VR has been around since the 1950s, although the term was coined in 1989 by Jaron Lanier, whose company manufactured the goggles and gloves used for the developing technology.
So what, exactly, is VR?
It is a simulated, three-dimensional environment that can be interacted with in seemingly real or physical ways using special electronic equipment, such as goggles with a screen inside or gloves fitted with sensors.
There are several types of VR, based on the level of immersion:
- Fully immersive VR places the user into a three-dimensional environment, often incorporating sound as well. Typically the user wears a headset or goggles with a screen and gloves with sensors, allowing interaction with the virtual environment around them. It is commonly used for gaming and entertainment, but is increasingly finding educational and therapeutic applications.
- Semi-immersive VR uses a partially virtual environment and is most often used for educational and training purposes.
- Non-immersive simulations are the most common kind of VR, forming the basis of most video game systems, like the Nintendo Wii and Microsoft’s Xbox. The user is in a physical environment, using a smartphone or a sensor device to interact with a virtual environment. These are often referred to as interactive video games.
In addition to VR, other digital technologies have been shown to be useful in physiotherapy, for example, smartphone and watch apps that count steps or track exercise or movement.
It’s all about engagement
Possibly the biggest advantage to using VR and interactive video games in the physiotherapy setting is engagement.
Physiotherapy relies on the client or patient completing their assigned exercise program for improvement to occur, and this is true whether a stroke patient is learning to walk again or an athlete is recovering from an injury.
As a lead investigator on the Activity and MObility UsiNg Technology (AMOUNT) trial conducted at the Institute for Musculoskeletal Health at the University of Sydney (Hassett et al 2020), Dr Leanne Hassett, APAM, says the engagement factor is a key advantage to using digital technologies in a therapy program.
‘If we think about rehab, patients need to do hundreds and thousands of repetitions to improve, to be able to stand, and walk, and just get back to their activities, and that’s a lot to expect people to do, just to stand up, sit down, stand up, sit down, again and again.

Leanne Hassett is investigating a range of digital technologies for use in neurological and aged care rehabilitation.
'This is a way to bring in some further enjoyment and gain some engagement with others, by playing some of the gaming systems with grandkids, for example, or competitions between patients on the ward or against the therapist who is working with them,’ Leanne says.
For Newcastle physiotherapist Craig Hewat, APAM, whose clinic Engage VR uses VR with its rehabilitation clients, engagement is the major factor in using the technology.
‘We know clients are a lot more engaged when they are in a gaming type environment—obviously they’re challenging themselves; it’s fun; they’re trying to beat their last score.
'But at the same time we’re getting them to work on their balance or their coordination, or the activity or fitness or whatever it may be.
'And that for me is huge,’ he says.
When working with paediatric clients, video games add fun to therapy regimens.
Paediatric physiotherapist Natasha Furmie, APAM, who provides VR-based physiotherapy via telehealth consultations and uses video games regularly with her young clients, says it’s an important aspect of her practice.
‘It is more fun for them.
'They don’t actually feel like they’re doing exercise; they don’t feel like they’re working.
'They’re practising skills to be able to do an activity.
'It’s almost like they’re just completing a game, but they’re actually working on their skills,’ says Natasha.
She says it’s especially useful for children on the spectrum, who may be quite introverted and don’t like playing sport or being around a lot of other people.
Ageless benefits and technical challenges
It might seem logical that younger people, both clients and clinicians, would gravitate towards using VR and interactive video game technology, but physiotherapists using the technology find it is embraced by all ages.
‘There’s this misconception that older adults may not be interested or want to use technology to support their care.
'But what I have seen is that all age groups across the life span have an interest in this type of technology if it has meaning to them and can be used in a way that they see has value,’ says Associate Professor Belinda Lange, a researcher at the Caring Futures Institute at Flinders University.
But there is a lot of variability in the types of technologies people use in their own time versus what they use in their practice.
‘We have been working with clinicians, asking about their perceptions of using technologies in clinical practice and their current clinical use.
'You would expect that perhaps some of the younger clinicians would feel more comfortable using different technologies and integrating them into practice.
'But we haven’t seen that come through,’ Belinda says.

Belinda Lange's research includes evaluating the use of immersive virtual reality for training and rehabilitation.
She is currently recruiting for a study exploring the awareness and use of technologies in allied health professions including physiotherapy (see the end of this article for more information).
Lusio Rehab is an Australian company that has developed a suite of video games for use in physiotherapy.
Paired with wearable sensors, the LusioMATE games can be played via a mobile device in the clinic or at home.
Clinicians can set up an individualised program for their patients and clients and work with them to play the games in the clinic.
They can also log in to see whether their patient is doing their exercise program at home and how they are progressing.
The platform is being used by physiotherapists for acute and chronic conditions as varied as stroke rehabilitation, chronic pain, spinal injuries, paediatrics, autism and musculoskeletal conditions and for fitness management, says CEO Justin Keenan, and has been developed in consultation with clinical partners.
‘A major feature in the platform is the inclusive environment,’ says Justin.
‘We have developed the technology so it can be used by anybody.
'Our sensors can be tailored for a very small range of movement.’
One of the biggest barriers to using VR and interactive video games in the clinic is getting started.
With so much technology entering the market, it’s hard to know where to begin.
‘I think it’s a benefit and a challenge, right?
'If you do the Google search and lots of things come up, you don’t know where to start.
'Until you try some of these technologies and see how they work for you, you’re stuck—it’s hard to imagine how you would use it in practice.
'I think that can be a sticking point for many people,’ Belinda says.
Leanne agrees, noting that there is a learning curve for the technology.
‘When a service or a physio is thinking about bringing a new technology in, they really need to make sure that they make time for learning how to use it, as well as keeping their skills up in being able to use it.
'It’s not just a one-off training session and then you’ll know what to do,’ she says.
It’s also necessary to make sure that there is adequate technical support for the systems in use, Leanne says, whether that is a tech-savvy physio or an IT support service or the platform’s technical support.
It’s particularly important if the technology is going home with the patient.
‘If the patient loses confidence, then they’ll just pack it away and not use it again,’ she says.
Cost is another factor that has to be taken into consideration.

Using the LusioMATE app, a patient does their exercises with the help of a physiotherapist (photo supplied by Lusio Rehab).
There is no one-size-fits-all package, so a variety of platforms and software might be required.
And older equipment may not work with newer apps and games.
‘The challenge as a business owner—more so than as a physio—is trying to keep up with the technology,’ Craig says.
Rather than buying off-the-shelf physiotherapy platforms, Craig and his team use a combination of commercially available hardware, software and games and have also been developing their own programs.
‘The IT guys will say this [game or software package] is great and I go, “Well, okay. It’s great but how can we use it clinically?”
'There’s a lot of games they’ll show me or things that they can do that are just not suitable for a clinical environment.
'From a hundred ideas I get, I probably use 30.’
Affordability is a big factor in the public health sector, says Leanne, and influenced the choice of technologies that were used in the AMOUNT trial.
‘Our technologies basically ranged from being free apps you could download to a couple of thousand dollars for a system that you would buy to be used in a rehab centre,’ she says.
Building the evidence base
While an evidence base is growing for using some of the technologies and apps in clinical practice, many of the studies tend to be small pilot studies, which don’t provide a lot of high-quality evidence.
Another challenge is the evolution of terminology for different technologies.
VR means different things to different people at different times.
Belinda is a co-author on a Cochrane review, first published in 2011 and updated in 2015 and 2018 (Laver et al 2018), which looks at the evidence for the use of VR and interactive video game consoles in stroke rehabilitation.
The review concluded that while there were some potential benefits, it wasn’t clear-cut, due to low-quality evidence.
Another Cochrane review on the use of VR in the treatment of Parkinson’s disease (Dockx et al 2016) came to a similar conclusion.
‘There’s some positive aspects and there’s great potential for the use of this technology, and we’ve seen that in a number of different areas, but I think there needs to be a more cohesive approach to look at larger studies that really focus on very specific types of interventions before we can truly look to the literature,’ Belinda says.
Ultimately, VR, augmented reality and interactive video game platforms will find their place as another tool in a clinician’s toolkit.
The opportunity is there to leverage that technology to support what physiotherapists do, to think differently about the approach to a clinical problem and to do things that might previously have been impossible.
‘Just like you might reach for a gym ball or TheraBand, you should be able to think about how you might use technologies in different situations with different people,’ says Belinda.
Gaming with kids
Natasha Furmie was not a gamer and had never played with VR before she started working for VR-based XRHealth as a telehealth physiotherapist in 2020.
‘Initially, it was a little bit daunting to put myself into something that I had never even done for fun, let alone for treating patients.

Natasha Furmie uses virtual reality as part of a telehealth package for paediatric clients.
'XR sent me a VR headset with the apps on it and I played around with it for a little while before I started treating clients to get myself familiar with it.
'I had to think, how would these actually help kids?’ Natasha says.
Most of Natasha’s clients are 8–16-year-old children with autism spectrum disorders.
She notes that the VR sessions are just one part of the telehealth package offered by XRHealth—she also works with the client and their family on other goals that are not addressed by VR apps.
While Natasha had never used VR prior to working with XRHealth, she wasn’t a stranger to the benefits of using video games.
In her full-time role at Sydney paediatric clinic Therapies for Kids, she uses physiotherapy video games, including the LusioMATE games, in her work with children.
Natasha says she uses the games not just directly for therapy, but to build a bond with her young clients, who come to the clinic with a variety of neurological conditions including cerebral palsy, autism spectrum disorders, Down syndrome and more.
‘I can know how to treat a condition inside out and back to front, but if that relationship is not developed with the child, you’re not going to get anything from them.
'So whether it’s telehealth, hands-on, VR, I’ve always spent the first three to four sessions developing a bond and I use what they love and what is their safe space.
'I use that to be welcomed into their world and then I become their physio,’ she says.
There are downsides, though.
VR and video games are not the answer to all problems, Natasha says.
There are a limited number of games available and after a while children get bored.
And then there are some things that just can’t be done with a VR app.
‘My focus area in paediatrics is higher-level disabled children and I work with them on things like head control, posture and the ability to sit or stand.
'It’s quite hard.
'There are no apps and there are no games that are targeted at that through VR; it is still very hands-on, physio based,’ says Natasha.
The engagement factor
Craig Hewat set up his physiotherapy clinic, Engage VR, with a major emphasis on using VR technology for rehabilitation of patients with brain and spinal cord injuries, stroke, Parkinson’s disease and other neurological conditions.
The practice incorporates VR into programs for clients alongside more traditional physiotherapy.
Craig says VR provides a perfect medium for encouraging neuroplasticity and the formation of new neural connections.

Craig Hewat uses virtual reality with rehabilitation clients in his practice.
‘We can put people under water; they can be flying; they can ride a unicorn; we’ve got so many different experiences where the brain is in an environment that it’s just not used to,’ he says.
Typically at Engage VR, clients are introduced to VR activities as part of their rehab program.
And although many of the clients at the practice are older, Craig says he hasn’t found age to be a barrier.
‘We’ve got 70, 80-year-olds in VR who think it’s the best thing they’ve ever done.
'But a highlight for me was a 96-year-old amputee who cried because one of the things he wanted to do in life was scuba-dive and we put him in VR swimming with whales.
'He thought it was the greatest thing he’d ever done in his life,’ Craig says.
Craig says the biggest benefit to clients is that often, they don’t even realise in the moment that they are exercising.
Being in a VR game environment can remove a level of self-consciousness, putting the therapeutic skill, such as balance, in the background.
‘They’re playing a game, they’re going to literally try and get their highest score, but at the same time they’re also doing therapy,’ he says.
VR is not just games, either.
It can be used to create relaxing landscapes such as beach scenes or forests for clients to experience as part of their therapy.
Craig says the results he has been getting in the clinic to date have been very positive.
He’s keen to see more evidence validating VR’s use in the clinic as well as evidence-driven development of games for specific injuries or conditions like Parkinson’s disease.
‘I’m biased but I do think it will become a part of what we do.
'I’ve been a physio for 26 years, involved in lots of areas of physio, and I can’t see myself working with these type of clients and not using it.
'The engagement factor alone is huge,’ Craig says.
Making rehab a game
At the Institute for Musculoskeletal Health in Sydney, the AMOUNT trial (Hassett et al 2020) looked at the use of a variety of digital technologies in the neurological and aged care rehabilitation setting.
Leanne Hassett says that the study was designed around the idea that rather than taking a one-size-fits-all approach, a range of technologies could be used to tailor interventions and therapy programs to suit the needs of the individual rehabilitation patient.
‘If you think about a rehab population, they’re quite heterogeneous, quite a mixed bunch of people,’ Leanne says.
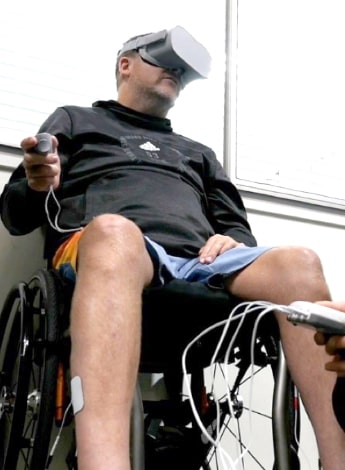
A patient uses VR under the supervision of a physiotherapist (photo supplied by Engage VR).
Leanne spent months playing with different digital technologies available to consumers, ranging from step counters like Fitbit to popular video game consoles including the Xbox Kinect and Nintendo Wii, as well as physiotherapy-specific platforms.
‘I think my kids thought I was secretly a gamer rather than going to work.
'I was looking at the games available and thinking about which ones were suitable for rehab.
'What mobility tasks could they be used for?
'Is there a way that you can modify the use of them so that they would be more suited for rehab?’ she says.
‘We ended up with eight different devices.
'We had four VR gaming systems.
'Two of them were the Xbox Kinect and the Nintendo Wii, and the other two were rehab-specific platforms—the Humac, similar to the Nintendo Wii Fit with a balance board, and another system called FysioGaming [from Netherlands-based company Doctor Kinetic], which was similar to the Xbox Kinect.
'Then we had wearable devices, which included Fitbits and Garmin watches.
'And we had some exercise and physiotherapy apps for the iPad,’ Leanne says.
A comprehensive intervention protocol allowed the physiotherapists to choose the device that suited both the patient and the therapy task.
As the trial progressed, patients moved from using the digital technologies in the inpatient rehab setting to using them at home.
Leanne says the trial results showed clinically and statistically important improvements in mobility that were maintained through the six months of the intervention and some positive outcomes of increased physical activity, such as self-reported walking.
Leanne says the patients really enjoyed using the digital devices as well.
One successful intervention session really epitomised the benefit of using the games.
‘I can clearly remember one participant, who was really slow at standing up and sitting down.
'And we pulled out one of the games from FysioGaming, which is a sit-to-stand game, and you’ve got to stand up and sit down to move a submarine up and down to catch the coins in the ocean.
'We went to show him this to say, “This is what we’re going to get you to do.”
'And he just started doing it, standing up and sitting down.
'So much fun and so much faster than getting through 70 more repetitions, because he was just doing what it was telling him to do, and he was engaged.’
Functional training in the virtual kitchen
Belinda Lange has built her research career around using digital technologies, including VR and augmented reality, to support rehabilitation and enhance training of allied health professionals.
She has evaluated the use of off-the-shelf gaming systems such as the Nintendo Wii Fit and Xbox Kinect as tools for physiotherapy, and worked in multidisciplinary teams to develop customised software and systems.
She is now working on several projects involving the use of immersive VR for rehabilitation and training.

Belinda Lange’s virtual kitchen allows users to make a cup of tea (photo supplied by Belinda Lange/Flinders University).
At Flinders University, where she is the research lead for Technology in the Caring Futures Institute (College of Nursing and Health Sciences), Belinda is working with an industry partner to design an interactive virtual kitchen to help with functional training in people with brain injuries.
‘In this virtual kitchen, you put on the headset and you can interact with any of the objects in the kitchen.
'But you can also set up different tasks within the kitchen, like cleaning out the refrigerator, making a cup of tea, making a sandwich,’ Belinda says.
While the project is still in its early stages, a pilot study compared a group of people with brain injury to a control group, looking at the differences between making a cup of tea and a sandwich in a real kitchen versus the virtual kitchen environment.
‘In the early stages of this research [we want] to see how we might be able to use this type of technology to support people to practise everyday activities in a meaningful way, but in a safe environment.
'We’ve been working with physios, but also OTs and speech pathologists and psychologists, as part of that project,’ Belinda says.
The beauty of the kitchen environment, she says, is that it spans a number of different needs for different allied health professionals, who might work together to treat a patient who has had a brain injury or a stroke.
‘You’ve got the physical interaction, but you’ve also got some of those cognitive elements.
'Like planning and attention; you can’t separate those and I think that’s really useful for both assessment and training,’ Belinda says.
Having a virtual environment also means that there is complete control over it.
The stimuli can be standardised for assessment or training purposes or adjusted to meet the needs of the patient.
Belinda’s team at Flinders University is also working on a number of other projects, including an art therapy environment and a ‘Buddy biking’ project with researchers at Aalborg University in Denmark.
In the latter project two cyclists work together in a virtual environment to ride a tandem bike.
While the bikes have devices on the pedals to measure the speed of pedalling, the interactions are less about competition and more about encouraging each other to keep the bike moving, she says.
Belinda is currently looking for physiotherapists and other allied health professionals to take part in a survey about their use of various technologies in clinical practice.
Email CFITechnology@flinders.edu.au if you are interested in taking part.
- References
1. Dockx K, Bekkers EMJ, Van den Bergh V, Ginis P, Rochester L, Hausdorff JM, Mirelman A, Nieuwboer A. Virtual reality for rehabilitation in Parkinson's disease. Cochrane Database of Systematic Reviews 2016, Issue 12. Art. No.: CD010760. DOI: 10.1002/14651858.CD010760.pub2. Accessed 07 September 2021.
2. Hassett L, van den Berg M, Lindley R.I, Crotty, McCluskey A, van der Ploeg H.P, Smith S.T, Schurr K, Howard K, Hackett M.L, Killington M, Bongers B, Togher L, Treacy D, Dorsch S, Wong S, Scrivener K, Chagpar S, Weber H, Pinheiro M, Heritier S, Sherrington C. Digitally enabled aged care and neurological rehabilitation to enhance outcomes with Activity and MObility UsiNg Technology (AMOUNT) in Australia: A randomised controlled trial PLOS Medicine 17(2): e1003029. https://doi.org/10.1371/journal.pmed.1003029
3. Laver KE, Lange B, George S, Deutsch JE, Saposnik G, Crotty M. Virtual reality for stroke rehabilitation. Cochrane Database of Systematic Reviews 2017, Issue 11. Art. No.: CD008349. DOI: 10.1002/14651858.CD008349.pub4. Accessed 07 September 2021.
© Copyright 2025 by Australian Physiotherapy Association. All rights reserved.





