
Closing the communication gap

The importance of communication and the need for providing culturally secure and safe healthcare for Aboriginal and Torres Strait Islander peoples is highlighted this month, with National Close the Gap Day on 17 March. We hear from the researchers behind ‘clinical yarning’, a conversational approach to communication between healthcare providers and their patients, and about a study investigating the benefits of implementing clinical yarning. Also, physiotherapists at a unique practice in Far North Queensland that takes physiotherapy out on Country talk about what makes the model so special. And with the release this month of the second series of the APA’s The Deadly Physios podcast, we learn how physiotherapy educators at the University of Melbourne are using the podcast as a teaching resource.
Yarning with purpose
Clinical yarning is a form of informal conversation that is increasingly being used by clinicians working with Aboriginal and Torres Strait Islander peoples to facilitate better communication with patients and clients.
Yarning is a form of ‘conversation with purpose’ in Aboriginal and Torres Strait Islander cultures.
Based on storytelling, it is an informal way to give and receive information that revolves around establishing a relationship between the participants and creating a culturally safe space.
And it’s increasingly finding a place in clinics that work with Aboriginal and Torres Strait Islander patients.
‘Yarning is a conversation.
'It’s an Indigenous form of conversation.
'You know, we’ve grown up learning how to use it,’ says Professor Dawn Bessarab, director of the University of Western Australia’s Centre for Aboriginal Medical and Dental Health.
Dawn, an Aboriginal woman of Bard (West Kimberley) and Yjindjarbandi (Pilbara) descent, has developed yarning frameworks for use in research and more recently for use in clinical environments, in collaboration with Geraldton-based physiotherapist Ivan Lin and his colleague Charmaine Green (Lin et al 2016).
The clinical yarning framework grew out of some teaching that Ivan and Charmaine were doing at the Western Australian Centre for Rural Health in Geraldton, where allied health and medical students of all kinds were learning how to interview Aboriginal patients, says Ivan, who recently became a Fellow of the Australian College of Physiotherapists.
‘We found that the students’ communication wasn’t very good.
'They were asking the right questions but they were firing questions at these poor community teachers.
'And the information they were getting was quite narrow,’ he says.
Ivan realised that they needed to come up with a better way to teach their students to talk to their Aboriginal patients.
To come up with a patient-centred framework for clinical yarning, Ivan and Charmaine turned to Dawn to adapt her research yarning framework to the needs of the clinic.
Research yarning includes four different types of yarning—social, research topic, collaborative and therapeutic.
These have been modified for a clinical situation to include social, diagnostic, management and therapeutic yarning.
The social yarn is an informal and unstructured conversation that helps to build a relationship between the clinician and the patient or client.
For Aboriginal and Torres Strait Islander people, this form of yarn establishes Country and relationships—who is your mob, where is your Country, Oh, you’re from there, do you know so and so?
In a clinical situation, the social yarn can be used to talk about common interests and other information that establishes a rapport between the participants.
Dawn says clinicians shouldn’t be nervous about talking to an Aboriginal client, even if they have never spoken to an Aboriginal person before.
‘They say, “Well, how can I have a social yarn, when I’m not Aboriginal or I can’t talk about culture?”
'And I say, “Yes, but do you like sport? Are you a gardener? Do you like food? Where do you come from? Are you Australian? What part of Australia?”
'There is always something where you can find common ground with an Aboriginal person.
'You don’t have to talk about your family groups or where you come from; you can talk about other things, but you have to listen.
'And we talk about the importance of cues.
'Because usually Aboriginal people will give you the cue and you can decide which direction you will take the yarn in, you know.
'But that’s if you’re listening and your head isn’t occupied with a whole bunch of other things going on so that you’re only half listening,’ she explains.
Once trust has developed, diagnostic yarning allows the clinician to talk about and identify the patient’s clinical problem as well as factors that may play a role in the diagnosis.
‘It’s about finding out why a patient is wanting to see you about their medical condition,’ says Dawn.
‘Once you’ve had the diagnostic or clinical yarn, you then move into the management yarn.
'What am I suggesting to the patients about managing their clinical or their health diagnosis or condition?’
The fourth kind of yarn, which can come up at any point, is the therapeutic yarn, which is a yarn where someone unexpectedly discloses something traumatic or intensely personal.
‘Sometimes in a conversation or a yarn, when you’re not expecting it, someone might make a disclosure.
'So, in research, someone might talk about being traumatised because of the stolen generation or they’re in domestic violence or they’ve been sexually assaulted or something like that,’ Dawn says.
‘It’s a traumatic experience that they might never have talked about before.
'And then, all of a sudden, you know, that’s not what you’re there for, but now that you’ve had this disclosure, how do you deal with that?’
Ivan says that when a disclosure comes up in a yarn, it’s important to direct the person to the right care as needed.
‘Usually, the first thing I’d say is, “Have you spoken to anyone else about this? Have you spoken to a GP? Have you spoken to anyone in the social/emotional wellbeing team here?”
'Sometimes people have, but often they haven’t.
'And if it’s of concern, then I would say, “Look, I really want you to talk to them. Can I talk to the GP about this?”’ he says.
Ivan says that it’s not just trauma that can come up as a disclosure.
Sometimes it’s to do with complicated factors that affect a patient’s ability to manage their condition.
‘In my practice, I’ve seen a lot of people with persistent pain.
'In most cases, it’s not straightforward; there are multiple factors and it’s complex.
'And even when people don’t have trauma and complicated lives, a lot of management is about encouraging self-management strategies.
'It’s understanding that person’s context and how you can adapt that to fit into the context of their lives.
'So it’s negotiating and just talking and coming up with some sort of plan,’ he says.
That plan may need to include identifying and facilitating other care, whether that is from the GP or from a social work team or a psychologist.
While physiotherapists aren’t trained to deal with mental health conditions, they can help the patient access other services.
‘Physios need to have the skills to be able to help direct that person to the sort of care that they need.
'It might be a case of “You told me your life is really stressful. You’ve told me you’ve got a lot on. You’ve told me that [the stress] coincides when this pain gets worse. So, I’m asking you, what sorts of strategies do you have to manage this? All this stress?”
'And people might say “nothing”, you know.
'Or they might say, “I go for a walk with my grannies” or something.
'And you’ll say, “Okay, well, how often do you do that?”
“Oh, I haven’t managed to recently.”
“Do you reckon you could try and do that a bit more?”’ says Ivan.
At the heart of the clinical yarning framework is the need to develop active listening skills, paying attention to body language and non-verbal cues that add layers of information to the conversation.
‘We know that active listening is talked about in communication and this is very much engaged listening.
'It’s validating.
'It’s reflecting.
'It’s listening in an engaged way.
'It’s showing empathy.
'Allowing that person to tell their story and then making a plan based on that,’ says Ivan.
Ivan says there is an assumption that clinicians are either good or bad communicators, which he says is true to a certain extent.
‘But with patient-centred communication skills, you can teach those skills to people.
'With clinical yarning, we talk about the social yarn, the diagnostic yarn, the management yarn—it’s all underpinned by a series of skills that clinicians can learn and then apply in the right context.
'It doesn’t mean you need to use all of those skills with every patient.
'It’s patient-led.
'It’s patient-centred.
'So you’re responding and guiding the conversation,’ he says.
Ivan and Dawn say that sometimes clinicians are reluctant to introduce clinical yarning due to the perceived time it can take.
‘We’ve shown that actually the social yarn can be a really quick segue into people’s issues, if you build that relationship.
'And it doesn’t have to take more than two or three minutes, even a minute.
'And if it’s going longer than that, then you’re actually getting caught up in the social yarn and not moving into why the patient is there,’ Dawn explains.
Another issue that comes up is that patients might not want to have a yarn for a variety of reasons.
‘Clinical yarning is one of the many tools that you can have in your clinical toolbox.
'Just because a person is Aboriginal, it doesn’t mean that you’ll go, “Oh, gee, I’m going to have a yarn with them now.”
'You’ve got to judge it when the person comes in, because sometimes, all they want is a diagnostic.
'They just want to get in and get out.
'They don’t want to sit down and have a yarn with you,’ Dawn says.
Other issues of cultural safety may also need to be taken into account, such as gender or age.
For example, an older Aboriginal man may be very uncomfortable speaking to a younger clinician or an Aboriginal woman may only want to talk to another woman.
The other important part of the yarning process is learning to relate and describe the clinical issues in a way that the patient understands.
Dawn says it’s important to use metaphors when explaining a complex medical situation such as diabetes or heart disease.
And she points out that, especially in rural and regional Australia, English is often an Aboriginal person’s second or third language.
‘We explain the importance of metaphors around getting into an Aboriginal person’s frame of reference and worldview and through a narrative and through a story.
'Which is why story is really an important part of clinical yarning; you can explain some really complex topics.
'But we also talk about language and being mindful of the use of biomedical language so that in the yarn, you’re not assuming that people understand what you’re talking about when you’re talking about a cardiovascular problem,’ she says.
Since developing their clinical yarning framework, Dawn and Ivan have worked with clinicians both in Western Australia and across the country to teach the basics of clinical yarning as part of cultural safety and security frameworks.
They have developed training resources, including videos that can be used in cultural safety and security programs and incorporated into clinical training programs, and are in the process of revamping an e-learning program.
‘When we do clinical yarning workshops, one of the principles is co-facilitation.
'So it must have an Aboriginal person as part of that facilitation process.
'And we also want to have someone from a clinical background.
'[So we are providing both] a cultural perspective and a clinical perspective,’ says Ivan.
‘If you think about people in a health service, often they’ll get cultural awareness training and some of the feedback is, “Yeah, that was good, but I don’t know what to do.”
'Clinical yarning is a way to act at an individual clinical level; it’s one way that you can put into practice culturally safe and culturally secure care.
'But in the end, it’s individual, it’s patient-led, it’s having some tools.’
Clinical yarning study shows benefits of approach
One group that Ivan worked closely with is based at the QIMR Berghofer Medical Research Institute in Brisbane.
There, the Aboriginal and Torres Strait Islander Health group has been conducting a study examining the use of clinical yarning by clinicians at pain clinics.
‘It’s an adaptation of cultural capability training developed in Queensland by Queensland Health and by Aboriginal and Torres Strait Islander people within that program, and adapted using the clinical yarning framework to develop a specific training program for pain specialists in the pain clinics,’ says Greg Pratt, who leads the Aboriginal and Torres Strait Islander Health research team at QIMR Berghofer.
The study used input from both patients and their families as well as clinicians to co-design and implement the clinical yarning training program to clinicians at three pain clinics located in Brisbane and in Townsville, with a lot of input and assistance from Julie Rogers and Jermaine Isua, both cultural capability advisers from Queensland Health who developed the Queensland Health Cultural Capability training.
While the evaluation and analysis of the program’s results are still ongoing, the initial data is encouraging, says Dr Christina Bernardes, the project manager for the study.
‘There was a significant difference from before training to after training.
'Clinicians reported improvements in their knowledge, confidence and ability to communicate more effectively with Aboriginal and Torres Strait Islander patients.
'The study aim was to equip clinicians with culturally sensitive communication skills.
'Now we are excited to follow up with how this training translates into practice,’ Christina says.
Dr Andrew Claus, a physiotherapist and researcher at the Tess Cramond Pain and Research Centre at the Royal Brisbane and Women’s Hospital, was one of the clinicians who took part in the study.
Andrew says that going into the training, many of the clinicians were unsure what to expect.
‘Once Julie was able to unpack the stories and the background and the context more for us, we really found it fascinating.
'The first clinician who volunteered to practise the social yarn was out of their comfort zone.
'We could see that each person drew on what they had just learnt from the previous experience so that collectively, with six or eight of us all in the room, we were all learning from each other really well.
'So it was a good exercise,’ he says.
Andrew says he is still unpacking the lessons learned from the training.
‘From a research perspective it sparked new questions.
'Surveys at the Tess Cramond Pain and Research Centre show that people who identify as Indigenous commonly report greater challenges than people who don’t.
'We hope to examine survey profiles at a national level, to understand the needs and then to inform models of care development in the years ahead.
‘I’m also just really pleased to have helped enable this with our clinicians.
'They gained so much from it.
'Like any clinic, we’re here for the client.
'No one likes the awkward feeling that they’ve missed something with the client that might have contributed to the client rescheduling appointments, failing to attend or not gaining from what we’re doing because it’s the wrong intervention for them,’ he says.
Greg says that because the training was part of a research study, it will be up to Queensland Health and its services to implement it more widely.
‘The resource is there for them to use and it now rests with the hospital and health services and also with the cultural capability team to take it up and use it as they see fit, locally or jurisdictionally,’ he says.
Greg also notes that while the training program they developed specifically addresses the use of clinical yarning by pain clinicians, their experiences in designing and implementing the program will be useful in other clinical spaces seeking to implement clinical yarning and cultural security training.
‘But I would suggest that there is a benefit in developing sensitive and appropriate training for each of the service sectors rather than just having a one-size-fits-all approach, because it’s not only about patients.
'Remember, this was essentially an intervention with clinicians, so this was about changing clinician behaviour through a training package to make them more sensitive and better communicators when it comes to working with Aboriginal and Torres Strait Islander peoples,’ Greg says.
After taking part in the training program and reflecting on the techniques he learned, Andrew also sees wider use in his clinical practice as a whole.
‘Yes, this is targeting the communication with Aboriginal and Torres Strait Islander peoples, but so much of what we learn by connecting there is going to feed into great clinical skills elsewhere as well.
'I think we’re seeing the pace of life getting quicker and quicker in so many areas and time invested for social connectedness is often diminished,’ he says.
‘We’re struggling to make the best clinical use of digital tools.
'But we all love to get the non-verbal cues, the whole body, all the communication and understanding of the person.
'These things really matter.
'Their context, what motivates them.
'I think that some of the skills from clinical yarning can improve communication with all of our patients.
'It is wonderful to get that really deep understanding when you’re dealing with complex and persistent problems.’
Taking physio to Country
Cairns-based physiotherapy practice Active Performance (AP) has a unique approach to working with Aboriginal and Torres Strait Islander clients.
In Far North Queensland, physiotherapy sessions with Aboriginal and Torres Strait Islander people sometimes take a different path from the typical clinical session.
There, physiotherapists from Cairns-based practice Active Performance take clients out to do their physiotherapy sessions on Country.

Physiotherapist Simon Morris with one of his clients in Aurukun.
They might take them fishing in a favourite spot, down to the beach to walk on the sand or back to their traditional land for a visit with family and friends.
It’s a unique way of practising physiotherapy that has grown out of the team’s work with patients with Machado-Joseph Disease among the Aboriginal community on Groote Eylandt in the Northern Territory, says Simon Morris, a senior physiotherapist who has been with AP for four years, after spending several years working as a physiotherapist in Papua New Guinea.
‘A lot of what we do in a clinical setting, we can do at home or on Country down at the beach or at the creek, so why limit ourselves to those areas when we could be a lot more effective and get a lot better continuity by taking it out of the clinic?’ says Simon.
‘It provides a really comfortable environment for the client and their family to engage and ask questions.
'When they’re in an environment that they’re comfortable with, they tend to open up a lot more, particularly over time as you share stories.
'You yarn about various different things and really build that relationship.
'I’ve found that the family members have been a lot more open about challenges that they face and are more open to discussions about ways that we can facilitate, and that they can facilitate their family members moving forwards and about other services that are potentially available for them.
'It just opens really healthy discussions, ultimately benefiting that client with a disability.’
Matt Hoffman is a young physiotherapist who joined AP in 2020.
A Woolwonga and Larrakia man from Pine Creek near Katherine in the Northern Territory, Matt is working mostly with the clinic’s Aboriginal and Torres Strait Islander clients.
This allows him to combine his cultural heritage with his professional life and to give back to the community.
He says it feels very natural to work with Indigenous clients in this way and it’s a big contrast to the formal clinical environments he worked in after graduating from university.
‘I was always trying to be very clinical and very professional and it felt really unnatural and was quite hard for me to do on a regular basis.
'In this job, every day is great and I don’t really feel like I’m working. It’s awesome,’ Matt says.
AP works with clients around Cairns and all the way up the Cape and across the Atherton Tablelands as well as in East Arnhem Land and Groote Eylandt in the Northern Territory.
Even Yarrabah, which is the nearest Aboriginal community to Cairns, is an hour’s drive away.
The majority of their Aboriginal and Torres Strait Islander patients are National Disability Insurance Scheme clients and many have had to move closer to larger towns like Cairns to access medical services, including dialysis, meaning they are away from their traditional lands.
And those who live on their traditional lands may be too disabled to easily move around and participate in the activities they most enjoy.

Working with a client on Country in Cairns.
Exercises can be tailored to the environment and the needs of the clients, Matt and Simon say, and the physiotherapists take massage tables and easily transported exercise equipment with them when they visit communities or go out on Country.
But how the sessions are structured depends on the client’s goals and interests.
Because of the way the National Disability Insurance Scheme allocates funding, the clients can have quite a lot of sessions and sometimes they build up.
This gives the physiotherapists the chance to take their clients out and make a day of it.
‘Obviously, we’re still trying to do our one-on-one sessions as well and make the most of their exercise and treatment.
'But every now and then, for a special occasion or at their request, we take them up the beach or go walking on their grandfather’s Country or go for a hike if they’re physically able and just need a little bit of assistance.
'We’ll take their support worker, who might pack a lunch for them for the day or things like that.
'It’s tailored to each person, really; each one’s a different experience,’ Matt says.
‘We use fishing quite a bit.
'Pretty much every one of our clients loves fishing.
'We go four-wheel driving onto the beach and then walk on the sand—not in the water; crocodiles everywhere.
'We take their four-wheel walkers down or take their family members down with us and we all just have a barbecue and do their exercises, things like that.
'It depends on the funding, but we have a heap of clients out there and some people only need 20 minutes of therapy.
'Other people need more.’
It’s not without its challenges, however, especially in creating a culturally safe environment for the clients.
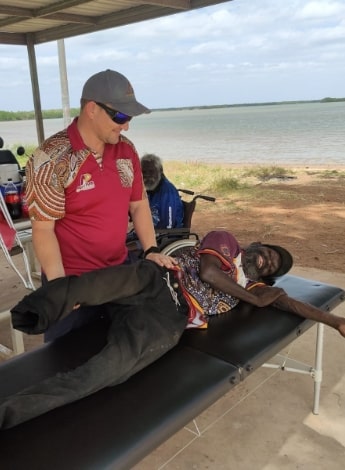
Physiotherapist Simon Morris treats one of his patients outside on Country in Aurukun.
Matt says that sometimes being a male physiotherapist treating female clients can cause a bit of discomfort, for example.
Currently, AP has no female physiotherapists, although there are female occupational therapists working at the practice.
‘You get the negative body language, different postures, things like that.
'It’s only sometimes; not everyone’s like that.
'Some of the older women are quite comfortable with male physios and other male health professionals treating them.
'But we’ve had quite a few ask for female physios or female allied health professionals to treat them,’ he says.
When this happens, Matt says, they work with the National Disability Insurance Scheme coordinator to come up with a solution that works for the client, such as having family members present during the session or teaching the exercises to a family member to work with the client.
Simon says he is not aware of any other practice in Australia that takes this approach in its work with Aboriginal and Torres Strait Islander patients.
‘We’ve looked around but we are yet to find anyone who’s doing a similar sort of model or similar sort of therapy.
'There might be some people seeing clients in homes, but generally when they’re flying out to community, whether it’s remote parts of Western Australia or the Northern Territory, even up in the Cape, they tend to be set up in a clinic and have the clients coming to see them there.
'One of the big things that I’ve found very common when speaking with physios who have done this is that they get very poor attendance rates; they might have 10 clients booked in for the day, but only two turn up,’ says Simon.
In contrast, he says, AP tends to have a really good attendance rate and continuity with the clients using their Physio on Country model.
From Matt’s perspective as an Aboriginal man, the model works because it is focused on making the client feel comfortable and valued.
‘It’s not Westernised.
'It’s looking at the client from a different perspective, taking a step back and looking at everything in the whole picture and trying to address all those cultural factors that are a bit different from a lot of the general public around here.
'Indigenous people, myself included—we don’t like going to clinics.
'Many have had a lot of bad experiences with clinics and just prefer being around their people and their community where they feel safe,’ he says.
‘I think a lot of businesses, physios and OTs know what they could be doing and what they should be doing with Indigenous people, but they just don’t think they can, because of how Western businesses and healthcare centres are set up.
'Because they’ve already made it a business that’s set in stone, they don’t really have the capability to go backwards and remodel it.
'Whereas this one has been well thought out, with a clear image in mind, and then built around that model.’
Clearly, the model works for the clients and the demand for AP’s services for Aboriginal and Torres Strait Islander clients has been increasing.
But just as importantly, the job is incredibly rewarding for Simon and Matt and their colleagues.
‘It definitely keeps you on your toes.
'It’s something different each day.
'You’re not really treating one thing at a time.
'It’s the whole person and they’ve got a lot of comorbidities you need to consider,’ Matt says.
Simon agrees.
‘My favourite thing being on Country is just seeing the client enjoy doing something that they haven’t done for a long time, whether that’s walking on the sand or into the salt water or into the creek.
'For some clients it’s fishing,’ he says.
‘It’s that enjoyment in seeing them—their face lights up when it’s something that means a lot to them that they haven’t been able to do for a number of years and it’s a pretty special moment and sometimes you’ve got family members in tears.’
Teaching students about truth-telling
Universities are using the APA’s The Deadly Physios podcast series as a resource for teaching physiotherapy students about reconciliation and Closing the Gap.
Physiotherapy educators at the University of Melbourne talk about how they have used the series to teach students about truth-telling.
Last year, physiotherapist Michael Reynolds recorded an episode of the The Deadly Physios podcast, talking about his personal journey as a Wiradjuri man and about the importance of truth-telling, which provides an opportunity for Aboriginal and Torres Strait Islander peoples to record evidence about past actions and share their culture, heritage and history with the broader community.
In the podcast Michael invites non-Indigenous Australians to engage in truth-listening as an extension to this concept and as a way for allies to engage with truth-telling.

Michael Reynolds, whose podcast episode on the art of truth-listening has been used as a resource for students.
His podcast is now being used by students in the University of Melbourne’s Doctor of Physiotherapy program as a resource for the seminar/Q&A panel discussion ‘Reflecting on the Triple Rs: Respect, Reciprocity and Reconciliation’, which forms part of the Healthcare in Context unit in their final year of study.
‘Michael’s podcast was used because he describes a way for non-Indigenous Australians and allies to engage with the learning and the storytelling, but also links it to Indigenous ways of knowing, which is deep listening,’ says Naomi Norris, lecturer for the Healthcare in Context course, which provides students with an understanding of the socio-politico-cultural influences on healthcare in a local and global context and of the development of skills in health promotion.
‘Michael’s invitation to non-Indigenous Australians to engage in truth-listening was central to what we were asking the students to do in the Reflecting on the Triple Rs seminar.’
The 2021 Reflecting on the Triple Rs seminar brought together a panel of Indigenous academics and physiotherapists and Indigenous allies, including APA President Scott Willis and APA Policy and Government Relations Advisor Lowana Williams, and The Deadly Physios podcast host and physiotherapist Cameron Edwards as well as Josh Cubillo, who is the Manager for Indigenous Programs in the Faculty of Medicine, Dentistry and Health Sciences, and the University of Melbourne’s Associate Director of Indigenous Strategy and Social Inclusion Margot Eden, the only non-Indigenous member of the panel.
Naomi says that the seminar is designed to deepen the students’ knowledge of Reconciliation Action Plans (RAPs) by looking closely at those of the APA and the University of Melbourne.
Each of the panellists talked about what the RAPs meant to them, professionally and personally, followed by a question-and-answer session with the students.
Michael’s podcast was provided to the students as a resource to help them think about deep listening and truth-telling in the lead-up to the seminar.
‘Engaging with Michael’s The Deadly Physios podcast really set the scene for what we were asking them to come into this space ready to do,’ Naomi says.
Healthcare in Context subject coordinator Jessica Lees says that part of the intent of the seminar was to encourage students to step out of their comfort zones to challenge their own biases.
‘One of our main aims is to embed Indigenous knowledge into our way of thinking.
'Part of truth-listening requires us to develop a knowledge of history and how it relates to place and the wellbeing of Indigenous peoples,’ Jessica says.
‘We’re not saying, “Okay, we’re reaching some end point with building culturally sensitive skills.”
'We want them to see it as a journey and we’re on that journey with them and encouraging them to be constantly building their skills in that space.’
The end goal, says her colleague Carolyn Cracknell, who is part of the team coordinating the program, is to take the students to a point where they understand that ongoing personal reflection, listening and learning are needed to provide culturally safe care and they take responsibility for this practice, even when it is not a comfortable space for them.
‘It is really about building into the lifelong learner skills.
'Part of that is being reflective and always challenging your biases and knowing why we need to do that, in particular when it comes to our First Nations’ health,’ says Carolyn.
Among the lessons imparted to the students is the message that having a RAP isn’t enough.
There needs to be support and belief driving it from within the organisation.
‘That was really caught by the students as well.
'The penny dropped and they understood that it’s not tokenistic as long as it’s not treated that way,’ Carolyn says.
‘The morning wasn’t all about saying, isn’t it great what we can achieve together in a positive frame?
'It was trying to say, we have a lot of healing to do and there’s a lot of truth-listening and action coming from that that needs to happen,’ says Naomi.
‘We talk a little bit about unlearning—those of us who are in positions of privilege, who have always been in the privileged part of society, actually have to unlearn a lot of things that we’ve taken as truths, because they’re not truths for everyone.’
Jessica says they received positive feedback from all of the seminar participants, with student comments such as ‘I look forward to embedding culturally safe practices into my physiotherapy DNA so that I may contribute to the restoration of trust in healthcare and closing the gap in health outcomes and life expectancies’ and ‘This experience has reinforced how proud I am to be part of a profession that takes action to improve the health and wellbeing of all Australians.
'I intend to utilise the RAP to inspire new ideas, create trusting relationships and champion for reconciliation with my colleagues.’
Ultimately, Naomi says, they want the students to understand that feeling uncomfortable in the face of truth-telling is part of the process of engaging in the conversation and recognising the need for cultural safety.
‘It’s actually about engaging in a practice as people and as professionals in order to keep providing culturally safe care going forwards and acknowledging that we all make mistakes along the way,’ she says.
Series 2 of The Deadly Physios podcast will be released on 17 March, which is National Close the Gap Day. Click here for Series 1.
- Reference
Lin et al (2016) ‘Yarn with me’: applying clinical yarning to improve clinician–patient communication in Aboriginal health care. Australian Journal of Primary Health, doi.org/10.1071/PY16051
© Copyright 2025 by Australian Physiotherapy Association. All rights reserved.





